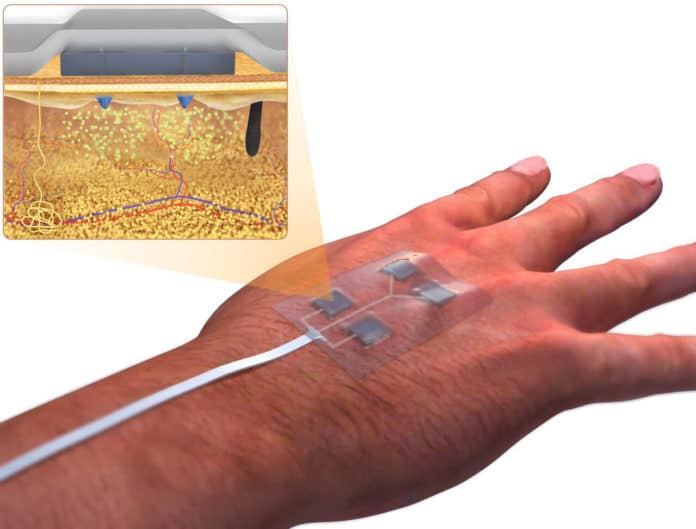
The treatment of the chronic and non-healing wound, which is also a major risk factor for diabetes-related lower-extremity amputation, usually involves the use of different drugs at different stages of the healing process. Every stage of healing requires a different kind of medication.
A team of researchers from UConn (University of Connecticut), the University of Nebraska-Lincoln, and Harvard Medical School has developed a “smart” bandage and corresponding smartphone-sized platform that can precisely deliver different medications to the wound with independent dosing.
This bandage is equipped with 3D printed miniature needles that – when activated by a smartphone-sized wireless controller – actively deliver a variety of drugs into deeper layers of the wound bed. The process is said to be fairly easy and painless.
This smart bandage can deliver that medication to the wound at the appropriate time. Also, it does not need to remove the bandage each time more medication needs to be administered. The wirelessly-controlled bandage allows the drugs to be programmed by care providers without even visiting the patient.
The team first conducted the research, published in the Advanced Functional Materials journal, on cells and later on diabetic mice with full-thickness skin injury. The animal’s wound was healed completely, with almost no scars, which shows the smart bandages’ ability to significantly improve the rate and quality of wound healing in diabetic animals.
The technology has the potential to replace existing wound care systems and change the way diabetic wounds are treated. According to the researchers, this method is more effective for wound closure, re‐epithelialization, angiogenesis, and hair growth when compared to the topical administration of drugs.
“This is an important step in engineering advanced bandages that can facilitate the healing of hard to treat wounds. The bandage does not need to be changed continuously,” says Dr. Ali Tamayol, associate professor at UConn.