Imperial scientists, in collaboration with the University of Edinburgh, have developed new software that can detect and quantify the severity of small vessel disease, one of the commonest causes of stroke and dementia. The software, which uses machine learning algorithms, can help clinicians administer the best treatment to patients more quickly in emergency settings and predict a person’s likelihood of developing dementia.
Small vessel disease (SVD) is an extremely regular neurological ailment in more established individuals that decreases the bloodstream to the profound white issue associations of the mind, harming and, in the end, slaughtering the cerebrum cells. It causes stroke, dementia, and, in addition, disposition aggravation. SVD increments with age yet is quickened by hypertension and diabetes.
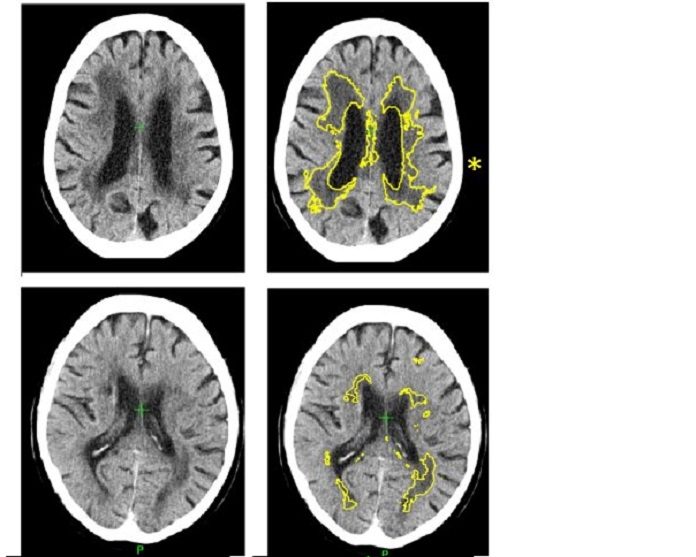
Doctors diagnose SVD by identifying changes in white matter in the brain during MRI or CT scans. But, in CT scans it is often difficult to decide where the edges of the SVD are, making it difficult to estimate the severity of the disease.
Dr. Paul Bentley, lead author and Clinical Lecturer at Imperial College London said, “This is the first time that machine learning methods have been able to accurately measure a marker of small vessel disease in patients presenting with stroke or memory impairment who undergo CT scanning. Our technique is consistent and achieves high accuracy relative to an MRI scan – the current gold standard technique for diagnosis. This could lead to better treatments and care for patients in everyday practice.”
“The importance of our new method is that it allows for precise and automated measurement of the disease. This also has applications for widespread diagnosis and monitoring of dementia, as well as for emergency decision-making in stroke.”
This software could help influence specialists’ decision-making in emergency neurological conditions and lead to more personalized medicine. For example, treatments such as ‘clot-busting medications’ can be quickly administered to unblock an artery in a stroke. However, these treatments can be hazardous by causing bleeding, which becomes more likely as the number of SVD increases.
It can also help quantify the likelihood of patients developing dementia or immobility due to slowly progressive SVD. This would alert doctors to reversible causes such as high blood pressure or diabetes.
During trials, the software analyzed identified and measured a marker of SVD and then gave a score indicating how severe the disease was, ranging from mild to severe. When compared with a panel of expert doctors who estimated SVD severity from the same scans, scientists found that the software is 85 percent accurate at predicting how severe SVD is.
The team is now using similar methods to measure the amount of brain shrinkage and other conditions commonly diagnosed on brain CT.
Journal Reference
- Liang Chen, Anoma Lalani Carlton Jones, Grant Mair, Rajiv Patel, Anastasia Gontsarova, Jeban Ganesalingam, Nikhil Math, Angela Dawson, Basaam Aweid, David Cohen, Amrish Mehta, Joanna Wardlaw, Daniel Rueckert, Paul Bentley. Rapid Automated Quantification of Cerebral Leukoaraiosis on CT Images: A Multicenter Validation Study. Neuroradiology. DOI: 10.1148/radiol.2018171567