In recent years, the emergence of innovative technologies made further advances in minimal access surgery possible. Advancements in machine learning, artificial intelligence, and imaging technologies will likely lead to even more precise and effective robotic surgery systems. It offers great potential for improving patient outcomes and enhancing the capabilities of surgeons.
In an exciting step forward in medical surgery advances, a surgical team from Washington University School of Medicine in St. Louis has successfully performed the first robotic liver transplant in the U.S. in May at Barnes-Jewish Hospital. The successful transplant extends to liver transplants and the advantages of minimally invasive robotic surgery.
The patient was a man in his 60s who required a critical transplant due to liver cancer and cirrhosis caused by the hepatitis C virus. According to the team, he is now doing well and has resumed normal daily activities. The patient was not only walking easily one month after surgery but was also looking to resume golfing and swimming. Typically, it would take at least six weeks for the patients to walk without discomfort.
“The transplant was a success: The operation went smoothly, the new liver started working right away, and the patient recovered without any surgical complications,” said transplant surgeon Adeel Khan, MD, the leader of the team that conducted the trailblazing surgery.
Washington University and Barnes-Jewish Hospital have been focused heavily on developing this cutting-edge technology as part of a concerted effort to advance minimally invasive surgeries and improve patient outcomes. Formed five years ago, the robotic transplant team has performed more than 30 robotic kidney transplants so far, all with good outcomes.
They also perform living-donor kidney removal surgery and other robotic surgeries involving the liver, bile ducts, pancreas, and stomach. But this is their and the nation’s first liver transplant.
“Liver transplantation is the most difficult of the abdominal organs to consider for a minimally invasive approach – given the difficulty of removing a failing liver and successfully implanting the new organ,” said William Chapman, director of Washington University’s Division of General Surgery and chief of the transplant surgery section.
Traditionally, a surgeon would make a 3- to 4-inch vertical and 12- to 16-inch horizontal incision just below the rib cage to remove a patient’s diseased liver and place the healthy donated liver. During the surgery to remove them, diseased livers are prone to excessive bleeding. Also, attaching the new liver to the patient’s circulatory system requires delicately sewing several tiny blood vessels together. This is why it had been thought to be too difficult to perform in a less invasive manner.
Robotic surgeries are a kind of minimally invasive surgery. During this successful robotic liver transplant, the surgeons operated through several half-inch keyhole incisions and made a single 6-inch vertical incision between the abdominal muscles to remove the diseased organ and place the new liver.
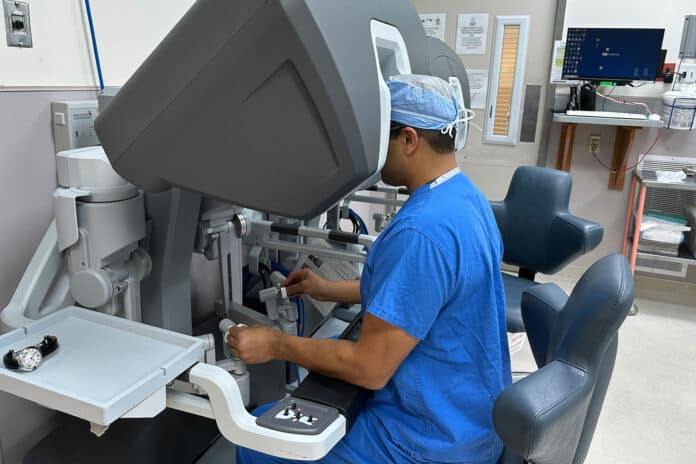
The eight-hour-long surgery was performed by advanced machinery, while the head surgeon controlled the robot’s movements from a screen nearby with joystick-like controllers. The large monitor displayed a magnified, 3D view of the surgical site, allowing for more precise and intricate surgery than traditional techniques.
Surgeons believe future robotic liver transplants likely will be completed faster as the team gains experience and gets more used to the subtleties of the new surgical technique.
“Further experience with this technique will be needed to establish the extent of the benefits of performing liver transplant as a minimally invasive approach,” Chapman said.