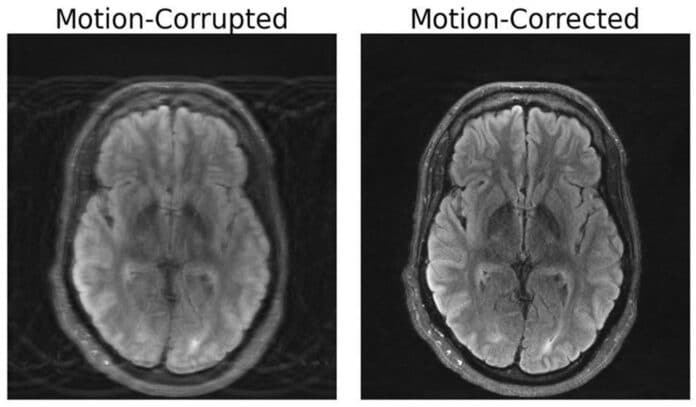
MRI scans offer high-quality soft tissue contrast over other imaging modalities such as X-rays or CT scans. But, they are more susceptible to motion, putting patients at risk of misdiagnoses or inappropriate treatment when critical details are obscured from the physician.
MIT scientists have come up with a solution to this. They have developed a deep learning model that can correct motion in brain MRI.
Without altering the scanning process, the method computationally creates a motion-free image from motion-corrupted data.
Through this, scientists aimed to combine physics-based modeling and deep learning to get the best of both worlds. Its importance lies in ensuring consistency between the image output and the actual measurements of what is being depicted, as failure to do so could result in “hallucinations”—images that appear realistic but are physically and spatially inaccurate, potentially worsening outcomes when it comes to diagnoses.
Nalini Singh, an Abdul Latif Jameel Clinic for Machine Learning in Health (Jameel Clinic)-affiliated Ph.D. student in the Harvard-MIT Program in Health Sciences and Technology (HST), said, “Future work could explore more sophisticated types of head motion as well as motion in other body parts. For instance, fetal MRI suffers from rapid, unpredictable motion that cannot be modeled only by simple translations and rotations.”
Daniel Moyer, an assistant professor at Vanderbilt University, said, “This line of work from Singh and company is the next step in MRI motion correction. Not only is it excellent research work, but I believe these methods will be used in all kinds of clinical cases: children and older folks who can’t sit still in the scanner, pathologies that induce motion, studies of moving tissue, even healthy patients will move in the magnet.”
“In the future, I think that it likely will be standard practice to process images with something directly descended from this research.”
Journal References:
- Nalini M. Singh, Neel Dey, et al. Data Consistent Deep Rigid MRI Motion Correction. arXiv. DOI: 10.48550/arXiv.2301.10365
- Jalal B Andre, Brian W Bresnahan et al. Toward Quantifying the Prevalence, Severity, and Cost Associated With Patient Motion During Clinical MR Examinations. J Am Coll Radiol. 2015 Jul;12(7):689-95. DOI: 10.1016/j.jacr.2015.03.007