Hypoxia, which occurs when cellular oxygen demand exceeds supply, is a common feature during inflammation associated with a bacterial infection. The reason for the occurrence of hypoxia during infection-associated inflammation is multifactorial and involves increased oxygen demand in order to satisfy the requirements of inflamed resident cells, infiltrating inflammatory cells, and, in some cases, multiplying pathogens.
Furthermore, chronic inflammation associated with long-term infection leads to the diminished blood supply to a tissue as a result of the combination of vascular pathology and microthrombosis. The combination of increased oxygen demand and decreased supply probably contributes to the hypoxia observed during infection.
In such a case, the body’s standard immune mechanisms, which rely on oxygen, can then only function to a limited extent. How does the immune system nevertheless manage to control bacteria under such conditions?
To find out the answer, scientists at the led by PD Dr. Anja Lührmann at the Institute of Microbiology – Clinical Microbiology, Immunology and Hygiene (Director: Prof. Dr. Christian Bogdan) at Friedrich-Alexander-Universität Erlangen-Nürnberg (FAU) and Prof. Dr. Jonathan Jantsch at the Institute for Medical Microbiology and Hygiene (Director: Prof. Dr. Dr. André Gessner) at University Hospital Regensburg infected macrophages with the obligate intracellular pathogen Coxiella burnetii, the causative agent of Q fever.
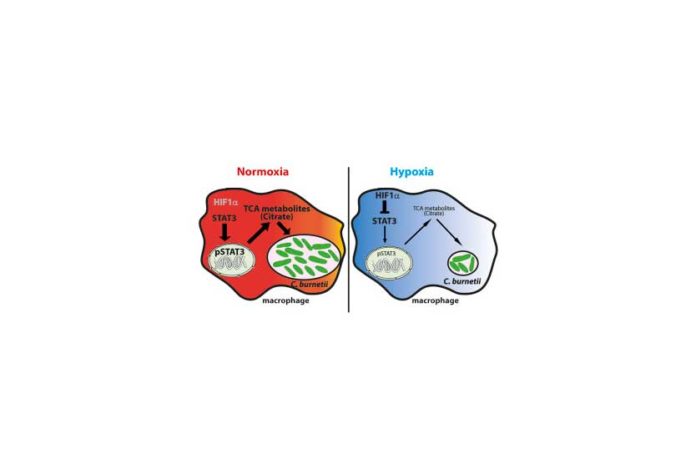
They found that fewer metabolites are produced in the citric acid cycle under hypoxic conditions, leading to a reduced rate of reproduction among bacteria in macrophages.
Scientists observed changes in the mitochondrial metabolism of the macrophages caused by signaling pathways initiated by the lack of oxygen (hypoxia). This leads to a reduction in various metabolites in the citric acid cycle, especially citrate. Also, it prevents bacteria reproduction, as citrate is an essential growth factor for certain bacteria.
Prof. Jantsch from Universität Regensburg. FAU scientist PD Dr. Lührmann said, “Our results describe a method of pathogen control which does not depend on oxygen and which we were not aware of until now. The pharmacological influence of these signaling pathways opens up new opportunities for fighting infectious diseases.”
The study is published in the journal Cell Press.