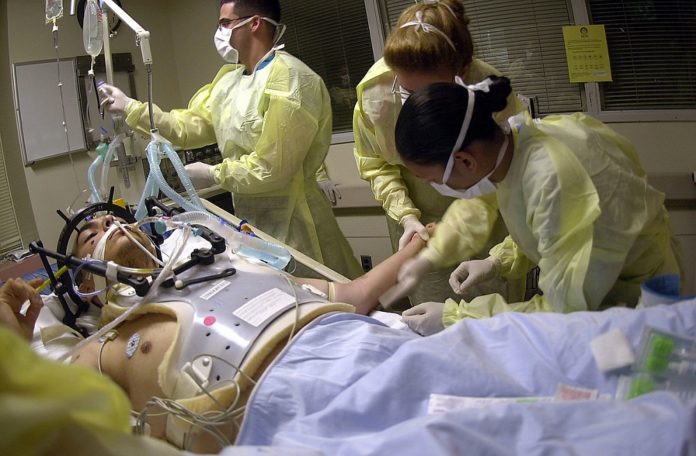
Contaminations in intensive care units (ICU) have a tendency to be caused by organisms, for example, multi-resistant gram-negative bacteria found in the gut, that are impervious to forefront anti-biotics. Treating such contaminations depending on expansive range anti-infection agents, which risk reproducing further drug-resistance, or antibiotics that have side-effects.
Evaluations of the extent of patients in ICU who will build up an optional disease range from one out of three to one out of two; around a half of these will be pneumonia. Notwithstanding, a few people are more susceptible than others to such diseases.
In a new study by the University of Cambridge, scientists have identified markers on three immune cells that correlate with an increased risk of secondary infection. These markers are expected to generate a ‘risk profile’ for an individual i.e., can offer a detail data on who is at greatest risk of developing a secondary infection.
The markers identified are found on the surface of key immune cells: neutrophils (frontline immune cells that attack invading pathogens), T-cells (part of our adaptive immune system that seeks and destroy previously-encountered pathogens), and monocytes (a type of white blood cell).
Scientists expect that this new test could help them fine-tune the choice of clinical trail members and enhance the trails’ chances of achievement.
The specialists tested the link of the presence of these markers with vulnerability to various bacterial and fungal infections. A person who tests constructive for every one of the three markers would be at a few times more greater risk of secondary infection contrasted and somebody who tests antagonistic for the markers.
The markers don’t demonstrate which secondary infection an individual may get, but instead that they are more vulnerable when all is said in done.
Professor Tim Walsh from the University of Edinburgh said, “As intensive care specialists, our priority is to prevent patients developing secondary infections and, if they do, to ensure they get the best treatment.”
Scientists noted, “A key part of enabling this study was to standardize how the research could be carried out across multiple sites. They used an imaging technique known as flow cytometry, which involves labeling components of the cells with fluorescent markers and then shining a laser on them such that they give off a light at different wavelengths. This has previously been difficult to standardize, but the researchers successfully developed a protocol for use, ensuring they could recruit patients from the four study sites.”
The study is published in the journal Intensive Care Medicine.