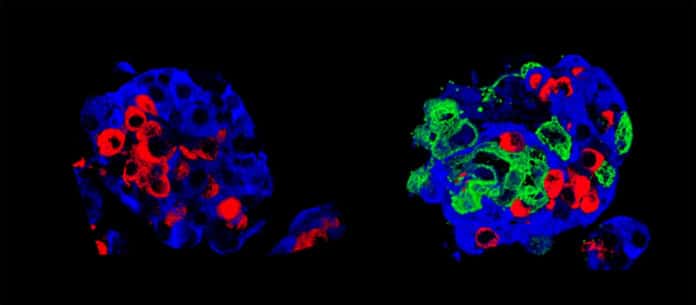
Type 1 diabetes happens when your immune system destroys cells in your pancreas called beta cells. They’re the ones that make insulin. The cell clusters in the pancreas called islets of Langerhans – where cells that produce blood glucose regulating hormones are grouped.
Pancreatic islet transplantation is an experimental treatment for type 1 diabetes. In this type of surgery, doctors take islets with healthy beta cells from the pancreas of a deceased organ donor. Doctors then inject the healthy islet cells taken from the donor into a vein that carries blood to the liver of a person with type 1 diabetes. These islets begin to make and release insulin in the recipient’s body.
However, this transplant procedure is long and complicated: a significant part of the grafted cells die quickly without being able to engraft. But now, scientists at the University of Geneva (UNIGE) and the Geneva University Hospitals (HUG), Switzerland, have found a solution to this. They have created much more robust “super-islets” of Langerhans by adding amniotic epithelial cells to these cell clusters.
Once transplanted, more of them engraft; they then start producing insulin much more rapidly. Scientists expect that the outcomes would not just improve the success of cell transplants, yet also, offer new viewpoints for different sorts of operations, including stem cell transplantation.
Scientists came up with a new idea of adding amniotic epithelial cells, taken from the wall of the inner placental membrane to the pancreatic cells.
Thierry Berney, Professor in the Department of Surgery at UNIGE Faculty of Medicine and Head of HUG Transplant Division, who co-directed this work, said, “These cells, very similar to stem cells, are already used in other therapies, such as corneal repair for example. In our case, we found that they can promote the function of pancreatic cells, which is to produce hormones according to fluctuations in sugar levels.”
Primarily, scientists added amniotic epithelial cells that allowed cell clusters to form regular spheres. This indicated better intracellular communication and connectivity. Later on, scientists transplanted their “super-islets” of Langerhans into diabetic mice, which quickly began to produce insulin.
Fanny Lebreton, a researcher in the Department of Surgery at UNIGE Faculty of Medicine, said, “Even with few cell clusters, our super islets adapted very well to their new environment and quickly became vascularized. A good vascularization is indeed the key element of any transplantation: it allows to supply the new organ with oxygen and nutrients and guarantees their survival. Also, the artificial islets quickly began to produce insulin.”
Ekaterine Berishvili said, “Amniotic epithelial cells are thus essential to islet survival and seem to act on two vital elements: the lack of oxygen, which usually kills a large number of transplanted islets, and the modulation of the host immune system to limit the risk of rejection. In any transplant, the first step is to lower the recipient’s immunity to limit the risk of rejection.”
“Amniotic epithelial cells have the unique characteristic of protecting the fetus, which is also a “non-self,” from attacks by its mother’s immune system. We believe that the same mechanism is at work to protect the grafts. The protective mechanism, observed here on cell transplants, could also take place in other types of transplants or even in xenotransplantation – where non-human cells or organs are transplanted into humans.”
The study is published in the journal Nature Communications.