A microbial sensor, Nod1, identifies bacterial infections and aids in developing blood stem cells, offering valuable insights. Raquel Espin Palazon’s team at Iowa State University discovered this, potentially eliminating the need for bone marrow transplants.
Published in Nature Communications, the finding builds on Espin Palazon’s earlier work, revealing the role of inflammatory signals in the embryo’s early stages and activating Nod1 in embryos forces vascular cells to become blood stem cells. This knowledge could pave the way for creating patient-specific blood stem cells derived from their own blood in the lab.
Espin Palazon said, “This would eliminate the challenging task of finding compatible bone marrow transplant donors and the complications that occur after a transplant, improving the lives of many leukemia, lymphoma, and anemia patients.”
Stem cells act as both the builders and raw materials in our bodies, constantly dividing to renew and create cells for different tissues. Embryonic pluripotent stem cells can become any cell type, while adult stem cells are limited.
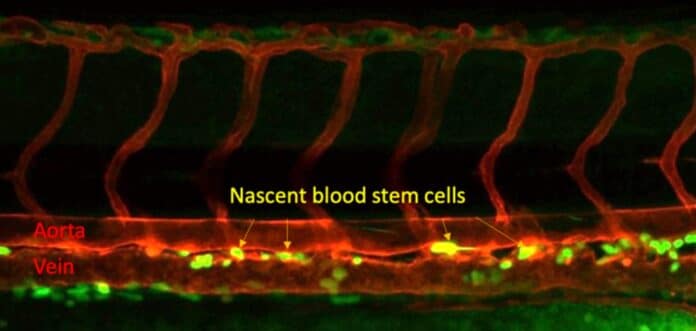
Blood stem cells, or hematopoietic stem cells, produce all blood components and are formed before birth in embryos. Raquel Espin Palazon’s team discovered an immune receptor that activates in embryos, preparing endothelial cells to become stem cells. This finding holds the potential for understanding and manipulating the creation of blood stem cells.
Raquel Espin Palazon said, “We know blood stem cells form from endothelial cells, but the factors that set up the cell to switch identity were enigmatic. We didn’t know that this receptor was needed or that it was needed this early before blood stem cells even form.”
Researchers identified Nod1’s role in blood stem cell creation by studying human embryos and using zebrafish. Nod1 levels are closely correlated with blood stem cell development. They collaborated with the Children’s Hospital of Philadelphia to validate this in humans, using induced pluripotent stem cells. Removing Nod1 hindered blood production, confirming its crucial role, similar to its impact on zebrafish blood stem cells.
Researchers, led by Raquel Espin Palazon, found that Nod1 is crucial for blood stem cell development. This discovery opens possibilities for creating blood stem cells from patients’ samples, a potential game-changer for treating blood disorders without needing bone marrow transplants.
The self-derived stem cells could mitigate risks like graft-versus-host disease. The ongoing research aims to understand the intricate timeline of blood stem cell formation, focusing on developing precise methods. Collaborating with the Children’s Hospital of Philadelphia enhances this effort.
The ultimate goal is therapeutic-grade blood stem cells for curing blood disorder patients. The study involves various Iowa State researchers and collaborators from the University of Edinburgh and Children’s Hospital of Philadelphia.
ISU researchers found a vital step in making blood stem cells. This discovery could create therapeutic-grade stem cells for treating blood disorders, offering a potential breakthrough in regenerative medicine.
The ongoing study focuses on refining methods and understanding the precise timeline of blood stem cell formation. Collaboration with the Children’s Hospital of Philadelphia enhances their efforts. The goal is to provide patients with a revolutionary option, using stem cells derived from their bodies, reducing risks associated with traditional treatments.
Journal reference:
- Cheng, X., Barakat, R., Pavani, G. et al. Nod1-dependent NF-kB activation initiates hematopoietic stem cell specification in response to small Rho GTPases. Nature Communications. DOI: 10.1038/s41467-023-43349-1.