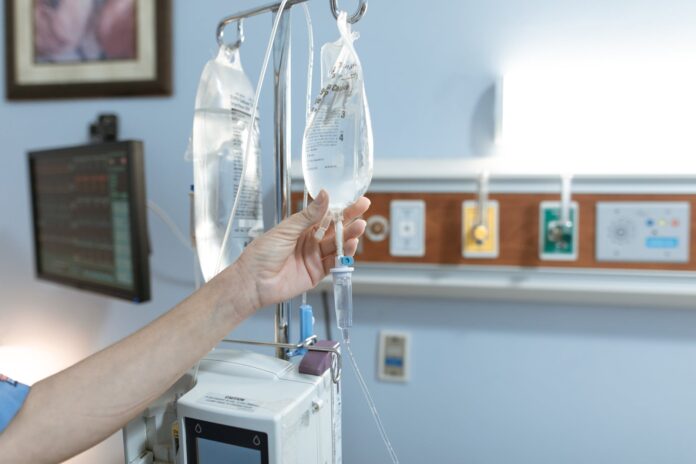
Sepsis is a leading cause of hospitalization, disability, and death worldwide. Despite improvements in the recognition and management of patients with sepsis, short‐term mortality in this group remains high. Survivors of hospitalization for sepsis remain at elevated risk of death and other adverse clinical events.
Cardiovascular disease (CVD) is increasingly recognized as a risk factor for and a potential consequence of sepsis. Prior studies have observed an association between sepsis and an excess hazard of late postdischarge CVD events; however, a recent meta‐analysis of observational studies found that the quality of evidence supporting this association was low because of the methodologic limitations of the published studies.
In a new study, scientists studied whether adults with sepsis may have a higher risk of death and a higher risk of rehospitalization for cardiovascular events after hospital discharge. Compared to patients who were hospitalized but did not have sepsis, those discharged after a hospitalization containing sepsis had a higher risk of cardiovascular events, rehospitalization for any reason, or mortality over a maximum follow-up of 12 years.
Researchers searched a database of administrative claims data. They discovered more than 2 million Medicare Advantage and commercial insurance members nationwide who had endured non-surgical hospitalizations lasting at least two nights between 2009 and 2019. Medical claims show that over 800,000 patients aged 19 to 87 had sepsis while hospitalized. Over a follow-up period from 2009 to 2021, the researchers examined the relationship between hospitalization and sepsis, rehospitalization, and death.
The researchers included the explicit and implicit sepsis diagnosis codes because discrepancies in sepsis diagnosis and documentation may impact study results and clinical treatment outcomes. When a patient has detailed sepsis, a doctor gives a formal diagnosis.
Implicit sepsis, the generally accepted definition, is an administrative code in the electronic health record automatically assigned when a patient has both an infection and organ failure. Patients were categorized as having sepsis vs. not having sepsis based on whether they met either criterion of sepsis.
To focus on the potential cardiovascular impact of sepsis, researchers compared 808,673 hospitalized patients who had sepsis to 1,449,821 hospitalized patients who did not develop sepsis but still had cardiovascular disease or one or more cardiovascular disease risk factors.
The findings suggest that compared to patients who did not have sepsis during their hospital stay, those with sepsis were 27% more likely to die, 38% more likely to be rehospitalized for any cause, and 43% more likely to return to the hospital specifically for cardiovascular reasons in the 12 years after having sepsis.
Lead study author Jacob C. Jentzer, M.D., FAHA, an assistant professor of medicine in the department of cardiovascular medicine at the Mayo Clinic in Rochester, Minnesota, said, “Our findings indicate that after hospitalization with sepsis, close follow-up care is important; and it may be valuable to implement cardiovascular prevention therapies with close supervision. Professionals need to be aware that people who have previously had sepsis are at very high risk for cardiovascular events and that it may be necessary to advise them to increase the intensity of their cardiovascular prevention.”
Journal Reference:
- Jacob C. Jentzer et al. Cardiovascular Events Among Survivors of Sepsis Hospitalization: A Retrospective Cohort Analysis. Journal of the American Heart Association. DOI: 10.1161/JAHA.122.027813