A team of international scientists led by Cortexyme, Inc., a privately held, the clinical-stage pharmaceutical company has recently discovered the role of a common bacterium, Porphyromonas gingivalis (Pg), in driving Alzheimer’s disease pathology. Through this study, they demonstrated the potential for small molecule inhibitors to block the pathogen.
Stephen Dominy, M.D., Cortexyme co-founder, a chief scientific officer said, “Infectious agents have been implicated in the development and progression of Alzheimer’s disease before, but the evidence of causation hasn’t been convincing.”
“Now, for the first time, we have solid evidence connecting the intracellular, Gram-negative pathogen, Pg, and Alzheimer’s pathogenesis while also demonstrating the potential for a class of small molecule therapies to change the trajectory of disease.”
Scientists identified Pg, the keystone pathogen in chronic periodontal disease, in the brains of mice with AD. They found that oral Pg infection leads to brain colonization. Moreover, it also increased the amyloid beta (Aβ) production. The amyloid beta (Aβ) is a key component of the amyloid plaques commonly associated with Alzheimer’s.
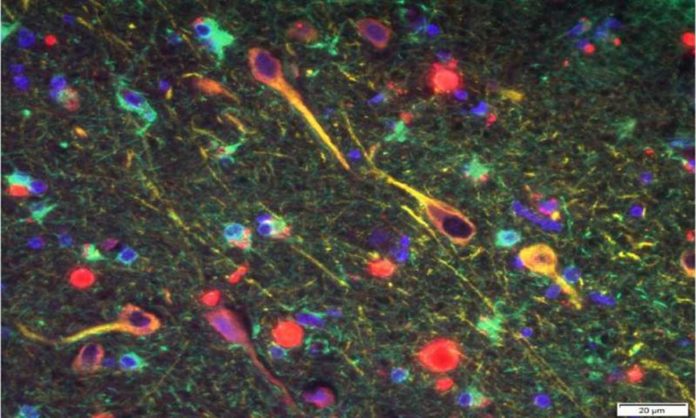
Scientists also detected the organism’s toxic proteases, or gingipains, in the neurons of patients with AD. The team correlated the gingipain levels with pathology related to two markers: tau, a protein needed for normal neuronal function, and ubiquitin, a small protein tag that marks damaged proteins for degradation and is found in tau tangles and Aβ plaques. The gingipains were found to be neurotoxic in vivo and in vitro, exerting detrimental effects on tau.
Seeking to block Pg-driven neurotoxicity, Cortexyme set out to design a series of small molecule therapies targeting Pg gingipains. In preclinical experiments detailed in the paper, the researchers demonstrated that inhibition by COR388, the most promising compound in the series and the subject of Cortexyme’s ongoing clinical development program, reduced the bacterial load of an established Pg brain infection, blocked Aβ42 production, reduced neuroinflammation, and protected neurons in the hippocampus, a part of the brain that mediates memory and frequently atrophies early in the development of AD.
Casey Lynch, Cortexyme‘s co-founder, chief executive officer, and an author on the paper said, “Despite significant funding and the best efforts of academic, industry, and advocacy communities, clinical progress against Alzheimer’s has been frustratingly slow. The publication sheds light on an unexpected driver of Alzheimer’s pathology—the bacterium commonly associated with chronic periodontal disease—and details the promising therapeutic approach Cortexyme is taking to address it with COR388.
In October 2018, Cortexyme announced encouraging results from its Phase 1b clinical trial of COR388 at the 11th Clinical Trials in Alzheimer’s Disease Conference. Investigators reported the compound was safe and well tolerated in healthy older volunteers and Alzheimer’s patients when given at a range of doses for up to 28 days.
COR388 was detectable in the cerebral spinal fluid (CSF) along with fragmented DNA from the bacterium that COR388 targets. Additionally, while the study was not powered for significance, COR388 showed positive trends across several cognitive tests in patients suffering from AD. Cortexyme plans to initiate a large Phase 2/3 clinical trial of COR388 in mild to moderate AD in 2019.
The study is published in the journal Science Advances.