During a conventional limb amputation, muscle movements are restricted, removing sensory feedback and causing it much harder for amputees to feel their prosthetic limbs are in space or to sense forces applied to those limbs.
During muscle contraction, other muscles don’t have their antagonist activity. As a result, the brain gets confusing signals.
Indeed, even with cutting-edge prostheses, individuals are continually visually following the prosthesis to attempt to calibrate their brains to where the device is moving.
A few years ago, the MIT Biomechatronics group had come up with a new amputation technique that maintains the relationships between muscle pairs. Their method involves connecting the two ends of the muscles to make them dynamically communicative within the residual limb.
A 2017 study of rats showed that when the animals contracted one muscle of the pair, the other muscle would stretch and send sensory information back to the brain.
In a new study, scientists develop a new type of amputation surgery that can help amputees better control their residual muscles and sense where their “phantom limb” is in space.
Scientists noted, “This restored sense of proprioception should translate to better control of prosthetic limbs, as well as a reduction of limb pain.”
Shriya Srinivasan, an MIT postdoc and lead author of the study, said, “Both our study and previous studies show that the better patients can dynamically move their muscles, the more control they’re going to have. The better a person can actuate muscles that move their phantom ankle, for example, the better they’re able to use their prostheses.”
In this study, scientists measured the precision of muscle movements in the ankle and subtalar joints of 15 patients who had AMI amputations performed below the knee.
These patients had two sets of muscles reconnected during their amputation: the muscles that control the ankle and those that hold the subtalar joint, which allows the sole to tilt inward or outward. The study compared these patients to seven people who had traditional amputations below the knee.
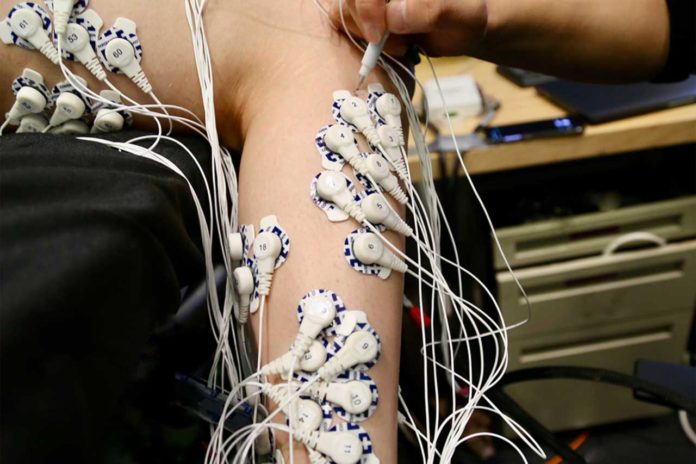
Patients did not wear prosthetic limbs during the study. Scientists asked them to flex their ankle joints — both the intact one and the “phantom” one — by 25, 50, 75, or 100 percent of their full range of motion. Electrodes attached to each leg allowed the scientists to measure specific muscles’ activity as each movement was performed repeatedly.
Later, scientists compared the muscles’ electrical signals in the amputated limb with those from the intact limb. They found that the electrical signals were very similar.
What’s more, patients with the AMI amputation were able to control the muscles of their amputated limb much more precisely than the patients with traditional amputations.
Srinivasan says, “The AMI patients’ ability to control these muscles was a lot more intuitive than those with typical amputations, which largely had to do with the way their brain was processing how the phantom limb was moving.”
“Our study wasn’t specifically designed to achieve this, but it was a sentiment our subjects expressed over and over again. They had a much greater sense of what their foot felt and how it was moving in space. It became increasingly apparent that restoring the muscles to their normal physiology had benefits not only for prosthetic control but also for their day-to-day mental well-being.”
Scientists also developed a modified version of the surgery. The process dubbed regenerative AMI can be performed on people who have already had a traditional amputation.
The process involves grafting small muscle segments to serve as the agonist and antagonist muscles for an amputated joint.
Hugh Herr, a professor of media arts and sciences, said, “We’re learning that this technique of rewiring the limb and using spare parts to reconstruct that limb is working, and it applies to various parts of the body.”
Journal Reference:
- Shriya S. Srinivasan et al. Agonist-antagonist myoneural interface amputation preserves proprioceptive sensorimotor neurophysiology in lower limbs. Science Translational Medicine, 2020; 12 (573): eabc5926 DOI: 10.1126/scitranslmed.abc5926