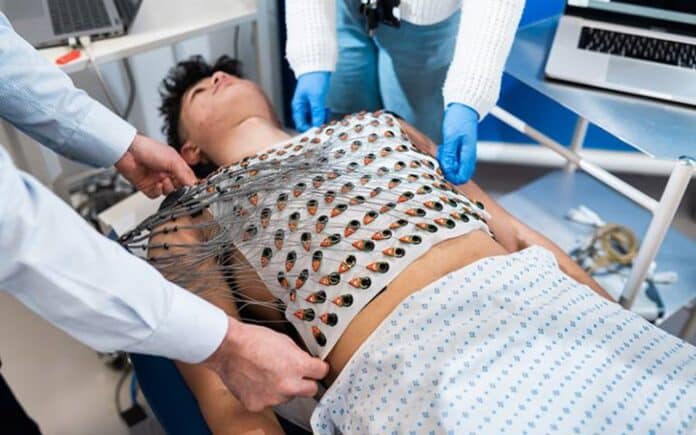
A study led by UCL researchers found that a reusable vest, capable of mapping the heart’s electrical activity in great detail, might help identify individuals at a higher risk of sudden cardiac death.
Our hearts beat because of electrical signals that regulate the heartbeat. When these signals go awry, it can lead to heart rhythm problems affecting two million people in the U.K., sometimes resulting in sudden death.
In the past, detailed mapping of the heart’s electrical activity was rare. It required invasive procedures or costly, time-consuming, and radiation-involved devices. However, a new electrocardiographic imaging (ECGI) vest developed by UCL researchers, detailed in a recent paper in the Journal of Cardiovascular Magnetic Resonance, is reusable and time-efficient. It can become a standard care tool, requiring only five minutes per patient.
The vest has 256 sensors that gather electrical data. Combined with detailed heart images from MRI scans, it creates 3D digital models of the heart and its electrical activity waves.
Dr. Gaby Captur from the UCL Institute of Cardiovascular Science and the Royal Free Hospital developed the vest with support from the British Heart Foundation (BHF) and the Society for Cardiovascular Magnetic Resonance. She pointed out that while heart imaging has advanced, monitoring the heart’s electrical activity has lagged. The standard tool, the 12-lead electrocardiogram (ECG), has mostly stayed the same for 50 years.
Dr Gaby Captur (UCL Institute of Cardiovascular Science and the Royal Free Hospital, London), who developed the vest with funding from the British Heart Foundation (BHF) and the Society for Cardiovascular Magnetic Resonance, said, “We believe the vest we have developed could be a quick and cost-effective screening tool and that the rich electrical information it provides could help us better identify people’s risk of life-threatening heart rhythms in the future.”
“In addition, it can be used to assess the impact of drugs, new cardiac devices, and lifestyle interventions on heart health. Currently, predicting the risk of sudden cardiac death is difficult, as it is not known, for instance, how risk might be affected by a particular structural feature or abnormality of the heart.”
Dr. Matthew Webber, a co-developer of the vest from the UCL Institute of Cardiovascular Science, explained that while cardiac MRI shows the heart muscle’s health, the vest’s electrocardiographic imaging adds a missing piece to the puzzle. It helps correlate features seen in MRI with their impact on the heart’s electrical system.
The researchers believe that improved risk assessment could assist clinicians in identifying individuals who may benefit from an implantable cardioverter defibrillator (ICD). ICDs monitor heart rhythm and deliver shocks if needed, potentially saving lives. However, they come with risks of infection and can be distressing if unnecessary shocks occur.
To confirm potential biomarkers obtained through ECGI for predicting risk, further studies tracking individuals over time are necessary to see if these biomarkers are linked to higher-risk outcomes.
The ECGI vest is reusable because it uses washable dry electrodes, unlike traditional metallic electrodes that need gel. It’s the first time such electrodes are used for ECGI. The vest’s feasibility was tested in 77 patients and proved reliable; it has since been successfully used in 800 patients, a significant increase from previous studies.
The vest is currently employed to map the hearts of individuals with conditions like hypertrophic cardiomyopathy and dilated cardiomyopathy. Dr. Captur has patented the vest in the U.S. with assistance from UCL Business and is collaborating with g.tec Medical Engineering GmbH, the prototype maker, to explore broader manufacturing possibilities.
The study underscores the potential of the heart vest in predicting sudden cardiac death risk by offering a comprehensive and reusable tool for mapping the heart’s electrical activity. The findings open avenues for further research, development, and potential integration into standard cardiac care practices.
Journal reference:
- Webber, M., Joy, G., Bennett, J. et al. Technical development and feasibility of a reusable vest to integrate cardiovascular magnetic resonance with electrocardiographic imaging. Journal of Cardiovascular Magnetic Resonance. DOI: 10.1186/s12968-023-00980-7.