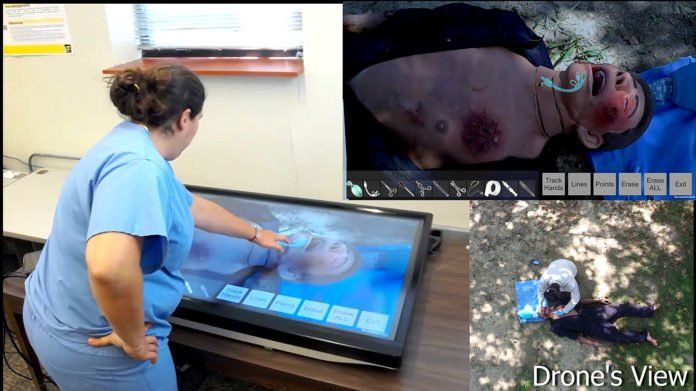
Purdue University analysts have built up a one of a kind approach that permits experienced specialists and doctors far and wide to help less-experienced doctors in war regions, natural disasters and in rural areas perform convoluted strategies.
The strategy utilizing augmented reality instruments to associate health care experts in remote areas with more experienced specialists and doctors worldwide. The AR headset worn by the mentee in the field is intended to supplant current telestrator technology, which utilizes a different video screen and freehand portrayals to give criticism.
Purdue’s James A. and Sharon M. Tompkins Rising Star Associate Professor of Industrial Engineering, who led the project team said, “The most critical challenge is to provide surgical expertise into the battlefield when it is most required. Even without having highly experienced medical leaders physically co-located in the field, with this technology we can help minimize the number of casualties while maximizing treatment at the point of injury.”
Edgar Rojas Muñoz, a doctoral student in industrial engineering, who worked on the project said, “There is an unmet need for technology that connects healthcare mentees in rural areas with experienced mentors. The current use of a telestrator in these situations is inefficient because they require the mentee to focus on a separate screen, fail to show upcoming steps and give the mentor an incomplete picture of the ongoing procedure.”
The headset screen display allows the mentee to see the patient in front of them, along with real-time on-screen feedback from the mentor. That mentor is at a separate location using a video monitor to see the AR feed and provide instant feedback to the field surgeon.
Moreover, the system uses computer vision algorithms to track and align the virtual notes and marks from the mentor with the surgical region in front of the mentee.
Muñoz said, “Our technology allows trainees to remain focused on the surgical procedure and reduces the potential for errors during surgery.”
The U.S. Department of Defense supported the research as it looks to connect its medical professionals out in the field with specialists back at the bases who can provide critical guidance during procedures.
The Purdue technology has gone through a round of clinical evaluation and will soon go through another one. In the next few months, the technology will be tested at a Navy base in Virginia, where mentees and mentors will experiment with a simulated battlefield.
The team presented the work at the 2018 Military Health System Research Symposium, held Aug. 20-23 in Kissimmee, Florida.