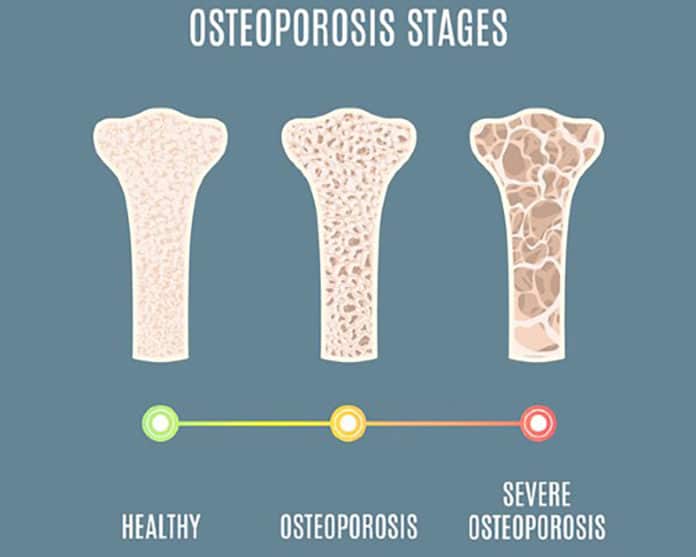
Osteoporosis is one of the most common musculoskeletal conditions in older people. Osteoporotic vertebral fractures (broken bones in the back due to osteoporosis) are significant because they identify people at high risk of future fractures.
Osteoporotic vertebral fractures (OVFs) identify people at high risk of future fractures, but less than a third comes to clinical attention despite this. To help address this important diagnostic care gap, academics at the University of Bristol have developed an online clinical checklist called Vfrac.
The tool helps health care professionals decide which older women with back pain should have a spinal radiograph.
Funded by Versus Arthritis, scientists carried out three relevant research studies in this area to identify triggers that could be used to identify who needs an X-ray. They also identified the changes in prediction accuracy when including self-reported back pain. They assessed the tool’s potential cost-effectiveness to establish whether to test it in a real-world situation.
1,635 women aged 65+ years were involved in the study. In the previous four months, these women self-reported back pain from nine GP practices in Bristol and 13 GP practices in Stoke-on-Trent. Exposure data were collected through self-completion questionnaires and physical examination, including descriptions of back pain and traditional risk factors for osteoporosis.
Scientists found that the tool correctly identified 70 percent of people with vertebral fractures. This is a significant improvement compared to the current 30 percent.
Descriptions of how back pain changed with activity – particularly increasing in a crescendo of pain when standing in the kitchen leaning slightly forward, such as how people stand when washing up – improved diagnosis of vertebral fractures. Health economic analysis strongly suggests that further testing of Vfrac is appropriate.
MMA Clark, Professor of Clinical Musculoskeletal Epidemiology at the University of Bristol, Consultant Rheumatologist and Consultant Rheumatologist at North Bristol NHS Trust (NBT), who led the research, said: “Vfrac can help healthcare practitioners decide which older women attending their GP with back pain are at high risk of currently having one or more broken bones in the back due to osteoporosis and need a diagnostic spine X-ray.”
“Our study found approximately one-third of people recommended to have X-rays by Vfrac will have a vertebral fracture. Virac identified more than 90 percent of severe vertebral fractures and approximately two-thirds of those with mild or moderate fractures. We now want to test Vfrac in a real-world clinic.”
Angela Davies, Head of Research Engagement at Versus Arthritis, said: “We are currently starved of the diagnostic tests needed for early detection, prevention, and treatment of musculoskeletal (MSK) conditions like arthritis and osteoporosis. Our research priorities and investments aim to significantly and decisively change this picture so that we can enter a world where MSK conditions can not only be treated but avoided.”
“This research chimes in with our ambition. Being able to test this tool in a clinical setting now brings us a huge step closer to supporting quicker diagnoses and ultimately better-targeted treatments for people with osteoporosis.”
Journal Reference:
- Tarnjit Khera, Linda P Hunt et al. A clinical tool to identify older women with back pain at high risk of osteoporotic vertebral fractures (Vfrac): a population-based cohort study with exploratory economic evaluation. DOI: 10.1093/ageing/afac031