In a new study, scientists from the National Institutes of Health conducted in-depth brain scans of COVID-19 patients. They spotted hallmarks of damage caused by thinning and leaky brain blood vessels in tissue samples from patients who died shortly after contracting the disease.
The surprising fact was there were no signs of SARS-CoV-2 in the tissue samples. It indicates that the damage was not caused by a direct viral attack on the brain.
The brains of patients who contract the infection from SARS-CoV-2 might be sensitive to microvascular blood vessel harm. The outcomes recommend that this might be caused by the body’s inflammatory response to the virus.
Avindra Nath, M.D., clinical director at the NIH’s National Institute of Neurological Disorders and Stroke (NINDS) and the senior author of the study said, “We hope these results will help doctors understand the full spectrum of problems patients may suffer so that we can come up with better treatments.”
COVID-19 is mainly a respiratory disease, but it also affects the brain. Patients often experience neurological problems, including headaches, delirium, cognitive dysfunction, dizziness, fatigue, and loss of the sense of smell. The disease may also cause patients to suffer strokes and other neuropathologies.
Several studies have shown that the disease can cause inflammation and blood vessel damage. In one of these studies, the scientists found evidence of small amounts of SARS-CoV-2 in some patients’ brains. Nevertheless, scientists are still trying to understand how the disease affects the brain.
This new study was conducted on brain tissue samples from 19 patients who had died after experiencing COVID-19 between March and July 2020. Samples from 16 of the patients were provided by the Office of the Chief Medical Examiner in New York City, while the department of pathology provided the other 3 cases at the University of Iowa College of Medicine, Iowa City.
The patients died at a wide range of ages, from 5 to 73 years old. They died within a few hours to two months after reporting symptoms. Many patients had one or more risk factors, including diabetes, obesity, and cardiovascular disease. Eight of the patients were found dead at home or in public settings. Another three patients collapsed and died suddenly.
For the study, a special, high-powered magnetic resonance imaging (MRI) scanner was used. The scanner is 4 to 10 times more sensitive than most MRI scanners.
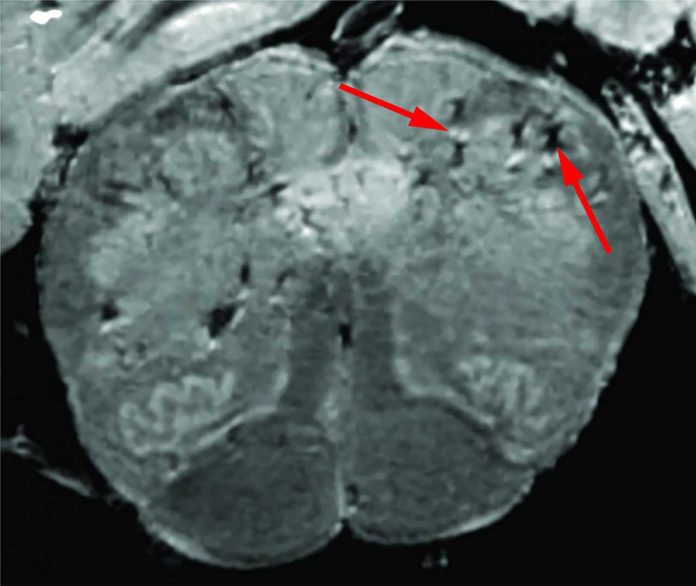
Using the scanner, scientists examined samples of the olfactory bulbs and brainstems from each patient. These regions are thought to be highly susceptible to COVID-19. The scans revealed that both regions had an abundance of bright spots, called hyperintensities, which often indicate inflammation, and dark spots, called hypointensities, represent bleeding.
Scientists then used the scans as a guide to examine the spots more closely under a microscope. They found that the bright spots contained thinner blood vessels than normal and sometimes leaking blood proteins, like fibrinogen, into the brain.
This appeared to trigger an immune reaction. The spots were surrounded by T cells from the blood and the brain’s immune cells called microglia. In contrast, the dark spots contained both clotted and leaky blood vessels but no immune response.
Dr. Nath said, “We were completely surprised. Originally, we expected to see the damage that is caused by a lack of oxygen. Instead, we saw multifocal areas of damage that is usually associated with strokes and neuroinflammatory diseases.”
“So far, our results suggest that the damage we saw may not have been not caused by the SARS-CoV-2 virus directly infecting the brain. In the future, we plan to study how COVID-19 harms the brain’s blood vessels and whether that produces some of the short- and long-term symptoms we see in patients.”
Journal Reference:
- Myoung-Hwa Lee et al., Microvascular Injury in the Brains of Patients with Covid-19, New England Journal of Medicine (2020). DOI: 10.1056/NEJMc2033369