Another examination demonstrates that stress quickens the advancement of pancreatic disease by setting off the arrival of “battle or flight” hormones. Beta blockers, generally utilized pharmaceuticals that restrain these hormones, were found to expand survival in a mouse model of the ailment.
An extra investigation of patients with cutting-edge pancreatic malignancy uncovered that the individuals who were taking beta blockers for another condition lived roughly 66% longer than the individuals who were not taking the solutions.
The examination, led by Columbia University Medical Center (CUMC) scientists, was distributed online in the journal Cancer Cell.
Late investigations have demonstrated that passionate and mental pressure assumes a part in the advancement of tumors as a rule. This impact is thought to happen through the thoughtful sensory system, which discharges hormones that give the body a surge of vitality so it can react to apparent perils.
Study leader Timothy C. Wang, MD said, “Some biologists dismissed this idea because stress is hard to measure. Others wondered how stress could possibly be related to a biological process that involves DNA mutations and the growth of cancer cells within a particular organ, such as the pancreas.”
The present examination was intended to discover the connections amongst push and early advancement of pancreatic malignancy. The scientists examined mice that are hereditarily inclined to creating strange developments in the pancreas. The mice were brought up in upsetting living conditions (restricted to a little space); control mice were brought up in ordinary lodging. Following 14 weeks, 38 percent of the focused on mice were found to have neoplastic pancreatic sores, a forerunner to pancreatic growth. No such injuries were seen in the controls.
Wang said, “We know that you need a DNA mutation to start on the path to cancer, but our findings suggest that stress is doing something to move things along.”
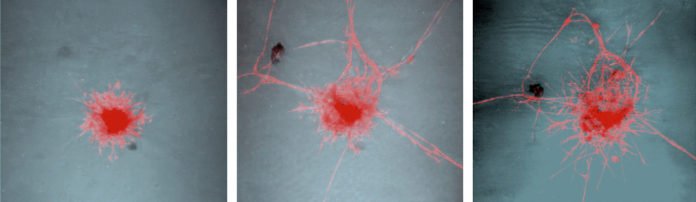
“That “something” was the subject of subsequent mouse experiments. These studies revealed that stress increases levels of catecholamines—the fight or flight hormones—in the bloodstream. Within the pancreas, catecholamines drive production of molecules that stimulate nerve growth around tumors.”
“Those new nerves, in turn, promote tumor development and make more catecholamines, perpetuating the cycle. “In other words, stress sets up what we call a feed-forward loop between nerves and cancer cells that promotes tumor development.”
In tries different things with an alternate mouse model of pancreatic cancer, the CUMC group showed that mice treated with chemotherapy and beta blockers lived essentially longer than mice treated with chemotherapy alone.
The scientists likewise took a gander at survival in 631 patients who had surgery in the vicinity of 2002 and 2013 to treat a progressed pancreatic cancer. The individuals who were taking nonselective beta blockers after surgery had a middle survival of 40 months, around 66% longer than patients taking specific beta blockers (which influence less focuses in the body) or neither kind of beta blocker.
Dr. Wang said, “It would be premature to recommend the use of beta blockers for these patients until we conduct prospective clinical studies, but beta blockers could potentially become part of the overall treatment regimen for pancreatic cancer.”
“A handful of studies and a lot of anecdotal evidence suggest that maintaining a positive outlook is good for your health and can help with recovery from almost any disease. Will a positive outlook change the prognosis of a patient with advanced pancreatic cancer? Probably not. But it certainly won’t hurt, and it could be part of the overall approach to slowing the progression of cancer to allow other types of therapy to kick in.”