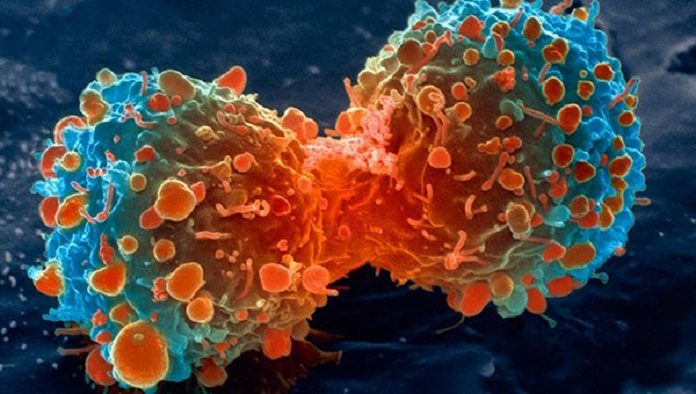
Circling tumor cells (CTCs) are little pieces of a tumor that split away and flow through the bloodstream. They contain an abundance of data about the tumor, for example, its compose, physical qualities and hereditary changes.
The capacity to rapidly and effectively reap and develop these cells from a blood test would empower “liquid biopsies” equipped for giving robust diagnosis, anticipation, and proposals for treatment techniques in light of individual CTC profiling.
CTCs are, extremely rare and difficult to catch. There are normally just a bunch for each couple of billion platelets going through a patient’s veins. While there are many technologies designed to separate tumor cells from normal blood cells, none of them are perfect. They tend to damage or kill the cells in the process, lack efficiency, only works on specific types of cancer or take far too long to be used in many situations.
In a new study, researchers from Duke University, MIT and Nanyang Technological University (Singapore) used sound waves, a universal group of analysts has built up a delicate, contact-free strategy for isolating circulating tumor cells from blood tests. It is fast and sufficiently productive for clinical utilize.
Using sound waves, scientists demonstrated a platform that is capable of separating CTCs from a 7.5-mL vial of blood with at least 86 percent efficiency in less than an hour.
Tony Jun Huang, the William Bevan Professor of Mechanical Engineering and Materials Science at Duke said, “Biopsy is the gold standard technique for cancer diagnosis. But it is painful and invasive and is often not administered until late in cancer’s development. With our circulating tumor cell separation technology, we could potentially help find out, in a non-invasive manner, whether the patient has cancer, where the cancer is located, what stage it’s in, and what drugs would work best. All from a small sample of blood drawn from the patient.”
The innovation works by setting up a standing sound wave at a point to a liquid coursing through a modest channel. Since sound is just a pressure wave, this sets up pockets of pressure that push on particles suspended in the liquid as they pass.
This acoustic power acts all the more unequivocally on the larger, more rigid cancer cells than on ordinary blood cells, pushing the CTCs into a different station for accumulation.
The power force and frequency of the sound waves are like those utilized as a part of ultrasonic imaging, which is utilized securely in various medical strategies. The risk of harm to the CTCs is decreased significantly promote on the grounds that every cell encounters the acoustic wave for just a small amount of a second and does not require naming or surface alteration. These highlights give the method the most ideal possibility at keeping up the capacities and local conditions of the CTCs.
Andrew Armstrong, associate professor of medicine, surgery, and pharmacology and cancer biology at the Duke University School of Medicine said, “The biggest asset of this acoustic method of separation is that it’s very gentle on the circulating tumor cells. The cancer cells remain viable after passing through the chip and can be characterized, cultured or profiled, which allows us to do genotyping or phenotyping to better understand how to kill them.”
“The idea is to develop personalized medicine approaches to individual patients based on their cancer biology, similar to what infectious disease doctors do with bacterial cultures and antibiotics.”
“The only FDA-approved technology for CTC detection can only count and do basic characterizations of CTCs but cannot grow CTCs outside of the body, because it basically kills the cells in the process. Being able to get to these cells while they’re still alive gives us at least a chance at culturing them or profiling them outside of the body to do the types of drug sensitivity and genetic testing that may better inform therapy.”
Scientists published their research in the journal Small.