In a recent study by the scientists at the Okinawa Institute of Science and Technology Graduate University (OIST) have analyzed three subtypes of depression. This is for the first time, scientists have identified depression sub-types from life history and MRI data.
And one out these 3 sub-types, one type of depression is by all accounts untreatable by Selective Serotonin Reuptake Inhibitors (SSRIs), a generally recommended medicins for the condition.
SSRIs, a commonly prescribed type of antidepressant, ease depression by increasing levels of serotonin in the brain. Serotonin is one of the chemical messengers (neurotransmitters) that carry signals between brain cells. SSRIs block the reabsorption (reuptake) of serotonin in the brain, making more serotonin available. SSRIs are called selective because they seem to primarily affect serotonin, not other neurotransmitters.
Prof. Kenji Doya said, “It has always been speculated that different types of depression exist, and they influence the effectiveness of the drug. But there has been no consensus.”
For the study, scientists gathered the data from 134 individuals – half of whom were newly diagnosed with depression and the other half who had no depression diagnosis– using questionnaires and blood tests. Scientists also asked about participants’ sleep patterns, if in case they had stressful issues or other mental health conditions.
Moreover, scientists scanned participant’s brain patterns using MRI. Through this technique, they examine 78 regions covering the entire brain, to identify how its activities in different regions are correlated.
Dr. Tomoki Tokuda, a statistician and the lead author of the study said, “With over 3000 measurable features, including whether or not participants had experienced trauma, we were faced with the dilemma of finding a way to analyze such a large dataset accurately.”
“The major challenge in this study was to develop a statistical tool that could extract relevant information for clustering similar subjects together. We thus designed a novel statistical method that would help detect multiple ways of data clustering and the features responsible for it.”
“Using this method, we identified a group of closely-placed data clusters, which consisted of measurable features essential for accessing the mental health of an individual. Three out of the five data clusters were found to represent different sub-types of depression.”
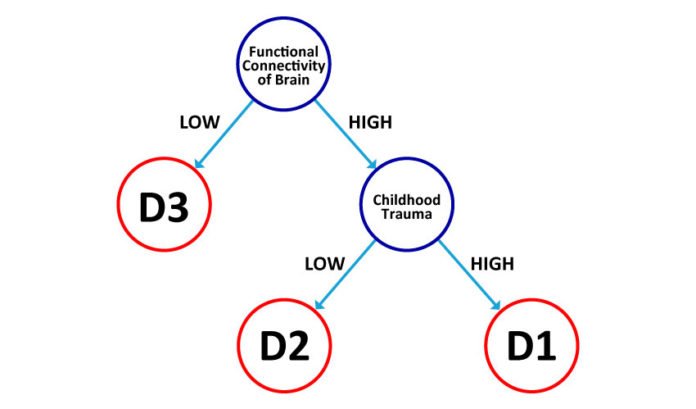
The three particular sub-sorts of depression were described by two principal factors: functional connectivity patterns synchronized between different regions of the brain and childhood trauma experience.
Scientists discovered that the brain’s functional availability in regions that included the angular gyrus – a brain region related with processing language and numbers, spatial cognition, attention, and different parts of cognition- assumed an expansive job in deciding if SSRIs were compelling in treating depression.
Patients with increased functional connectivity between the brain’s different regions who had also experienced childhood trauma had a sub-type of depression that is unresponsive to treatment by SSRIs drugs. On the other hand, the other two subtypes – where the participants’ brains did not show increased connectivity among its different regions or where participants had not experienced childhood trauma – tended to respond positively to treatments using SSRIs drugs.
Though, the study also identified some underlying factors and points to the need to explore new treatment techniques. In other words, it offers insights on neurobiological aspects of depression, so that scientists can pursue their research.
The study is published in the journal Scientific Reports and conducted with colleagues at Nara Institute of Science and Technology and clinicians at Hiroshima University.