Previously scientists have developed artificial blood vessels using sheepskin cells into a special tube. These artificial blood vessels have the ability to replace real blood vessels. But the method uses to create such kind of blood vessel is too complicated. So, to make the method less complicated and inexpensive, scientists from the Syracuse University have created model blood vessels.
These model blood vessels use 3D printing-enabled casting method that makes it more efficient, and precise. It has the ability to establish multiple cell layers in the channels.
Assistant Professor Pranav Soman said, “Most of the approaches to creating model blood vessels have been to mix a hydrogel with cells and relevant growth factors—the idea being that the cells and growth factors will automatically know to form microvessels. They do form networks and blood vessels, but they are randomly formed and don’t connect with each other.”
In reality, Syracuse University does not have a clean room. So, scientists need to work at other universities.
Scientists found 3D method too efficient in the manufacturing process. So, they used 3-D printing to create the mold that is essential to create the exact shape of these model blood vessels.
Soman said, “Off-the-shelf 3-D printers can cost between $1,500-2,500. Within that range, you can basically print anything you want as compared to a clean room that will cost thousands of dollars to get the work done.”
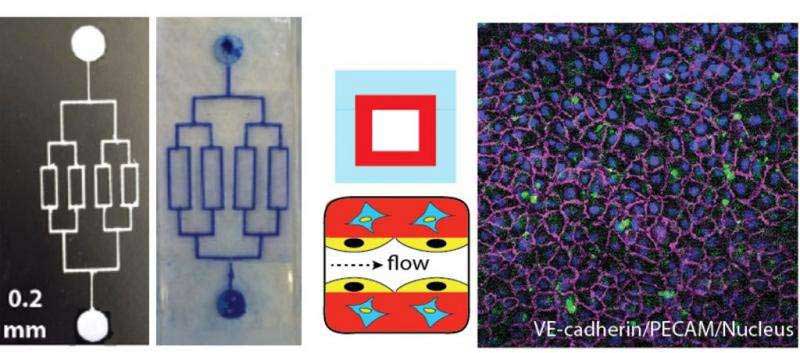
During experiments, scientists created an L-shaped channel from a mold created from a 3-D printer. There is a gel mixture spread on top of the mold. The gel consisting gelatin and vascular cells. In addition, the ultraviolet (UV) light is projected on it. When the liquid gel reacts to the UV, and it turns to a solid gel. The channel is then peeled from the mold.
Soman said, “Typically when these microfluidic vascular chips are made, they only have one layer of cells. But blood vessels inside the body are made up of three to four different cell types. The innermost cells, endothelial cells, are the ones that come in contact with blood, but the other layers of cells assist those inner cells.”
“If there is an injury or a blood clot, there is a whole reaction that takes place between these cells.”
“We have the ability to make two, three, four layers of cells with the same approach, so now you can capture the whole dynamic of what is happening between these different cell types and the endothelial cells. Before this, most chips use only the endothelial cells, so they have no idea what the other cells surrounding them may be doing in the context of clot formation or if there is injury or to simply understand fundamental vascular function.”
“If I want to study a branch or certain shape of an artery, I can print that shape, test the flow, and see where a clot will form—and maybe how can we prevent it and make new drugs to make sure a clot won’t get stuck.”
“Bone also requires a blood supply, so if I want to build a bone, I would want to make the small pipes of blood supply and fill with oxygen and other nutrients so that we can grow a large-scale 3-D bone. So one day we could potentially use in humans and replace a defective part of the bone completely. But to do that we have to understand the relationship between bone formation and blood flow. This vascular chip will enable us to study the interaction between the flow of blood and vascular cells and bone cells.”