COVID-19, caused by SARS-CoV-2, enters the human body through its spike protein, which attaches to a specific receptor in our cells. It mainly uses a protein called the angiotensin-converting enzyme 2 (ACE2) receptor to enter human cells. Lung cells have high levels of ACE2 receptors. That’s the reason the disease primarily infects the lungs.
In a new study, scientists from the University of Sydney have identified a protein in the lung that acts as a natural barrier to COVID-19. They found that a protein called leucine-rich repeat-containing protein 15 (LRRC15) in the lungs can block SARS-CoV-2 infection.
Like ACE2, the virus can also bind to a receptor called LRRC15. But unlike ACE2, LRRC15 does not support infection. It can, however, stick to the virus and immobilize it. While doing so, it protects other cells from being infected.
LRRC15 can be found in many organs like the lungs, skin, tongue, fibroblasts, placenta, and lymph nodes. But, a new study suggests that the lungs light up with LRRC15 after infection. It controls antiviral responses and fibrosis and could link COVID-19 infection with lung fibrosis during long COVID.
While blocking COVID-19, the receptor simultaneously activates the body’s anti-virus response and suppresses the body’s fibrosis response.
The study could potentially lead to the developing of new drugs to prevent viral infection from coronaviruses like COVID-19 or deal with lung fibrosis.
Professor Greg Neely from the Unversity of Sydney said, “For me, as an immunologist, the fact that there’s this natural immune receptor that we didn’t know about, that’s lining our lungs and blocks and controls virus, that’s crazy interesting.”
“We can now use this new receptor to design broad-acting drugs that can block viral infection or even suppress lung fibrosis.”
Dr. Lipin Loo, a postdoctoral researcher, said, “We think it acts a bit like Velcro, molecular Velcro, in that it sticks to the spike of the virus and then pulls it away from the target cell types.”
“The virus is coated in the other part of the Velcro, and while it’s trying to get to the main receptor, it can get caught up in this mesh of LRRC15.”
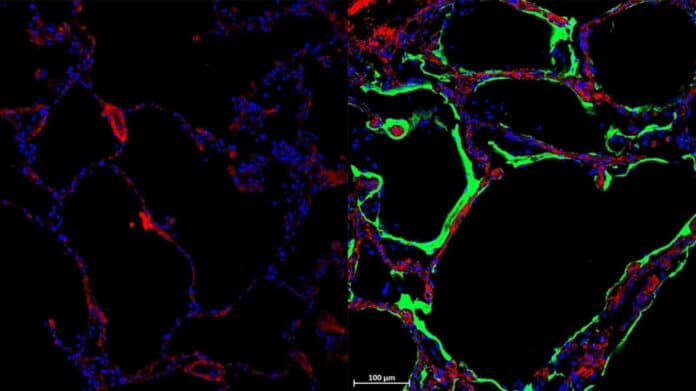
“When we stain the lungs of healthy tissue, we don’t see much of LRRC15, but then in COVID-19 lungs, we see much more of the protein.”
“We think this newly identified protein could be part of our body’s natural response to combating the infection, creating a barrier that physically separates the virus from our lung cells most sensitive to COVID-19.”
Scientists are now using LRRC15 to develop two strategies against COVID-19: one which targets the nose as a preventative treatment and another aimed at the lungs for serious cases.
Dr. Loo said, “The presence or lack of LRRC15, which is involved in lung repair, is an important indication of how severe a COVID-19 infection might become.”
“A group at Imperial College London independently found that the absence of LRRC15 in the blood is associated with more severe COVID, which supports what we think is happening. If you have less of this protein, you likely have serious COVID. If you have more of it, your COVID is less severe.”
Journal Reference:
- Lipin Loo, Matthew Waller, et al. Fibroblast-expressed LRRC15 is a receptor for SARS-CoV-2 spike and controls antiviral and antifibrotic transcriptional programs. PLOS Biology. DOI: 10.1371/journal.pbio.3001967