Drug resistance may not be the only reason for a drug failing to treat properly or losing its proven effectiveness. Poor quality of the drug might also be contributing to decreased effectiveness. This is what researchers have found in the case of a drug used to treat ringworm infection.
Doctors from the department of dermatology at the Dr. Ram Manohar Lohia Hospital (RML), New Delhi, have found quality issues in the drug being sold under various brand names for the treatment of ringworm infection. The drug in question is Itraconazole (ITZ), which has been in use for a long time.
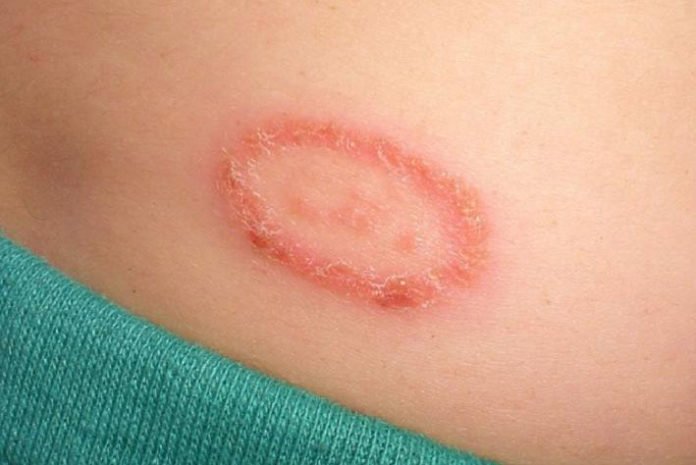
Ringworm (tinea or dermatophytosis) is a type of fungal infection of the skin which can affect both humans and animals. It can occur anywhere on the body including scalp, feet, groin, and beard. The name ringworm is a misnomer because the infection is caused by a fungus and not a worm. The infection is treatable with antifungal medications like ITZ.
However, of late, some brands of ITZ have been showing decreased effectiveness against ringworm infection, even when given in high dosage. Researchers, therefore, wanted to know if the problem was due to drug resistance or quality of drug being sold in the market.
When asked what made them carry on their study on the quality of the drug, Dr. Kabir Sardana, a member of the research team, said: “the possibility for drug resistance had been ruled out in an earlier study a team member so we thought the other cause should be quality of the drug.”

ITZ is available as capsules with drug-coated pellets inside. The pellets improve bioavailability by providing large surface area for absorption. According to researchers, the size and number of the pellets are important and they have to meet the desired specifications. A quality drug should have a large number of pellets with a smaller size.
The researchers analyzed 21 most commonly prescribed brands of 100 mg capsules of ITZ along with the innovator drug which is USFDA–approved, based on the number of pellets, their size, and cost. They found the innovator drug had pellet count of 820 and size of 969 micrometres. Of 21 other drugs, only three were found to have a pellet number of more than 600 while three had less than 300 pellets per capsule. A few brands were found to contain only dummy pellets and loose powder within the capsule.
As for the size of pellets, the researchers found it to vary, on an average, between 959 micrometer and 1845 micrometer. The cost of 100 mg capsule also varied widely. While the innovator drug costs Rs. 81 per capsule, cost of other brands ranged between Rs.9 and Rs.81.
“A wide variation (in the size) of pellets was seen and this is a downstream indicator of the manufacturing quality,” explained Dr. Sardada.“If the size and number of pellets are not maintained to the optimum level, benefits of the drug are likely to get affected.”
At the same time, researchers said, a cost cannot be taken as a surrogate of better quality because it was found that some brands were much cheaper than their costlier counterparts from multinational companies. However, as a way forward, further research is needed to assess the quality of ITZ. “We are undertaking further laboratory-based work to assess the quality of the drug, which in view of the rising resistance to terbinafine in India is our last bet for this India-centric problem,” said Dr. Sardana.
The findings have been published in Indian Dermatology Online Journal. The research team included Dr. Kabir Sardana, Dr. Ananta Khurana, Dr. Ajeet Singh, and Dr. R. K. Gautam.