Breast cancer (BC) is a complex disease comprising multiple distinct subtypes with specific genomic and pathological characteristics. Currently, a variety of medications are accessible for the treatment of breast cancer.
However, because the disease is so complex, only some benefit from the same medications. DNA sequencing can teach a little bit about the type of treatment that will be most beneficial for a patient. Therefore, better approaches are required to forecast how patients will respond to treatment because it is frequently impossible to say whether a treatment will benefit the specific patient.
A technique developed by scientists at Karolinska Institutet might be able to predict whether a breast cancer patient will benefit from a specific treatment or not. The cell-based approach has been tested on patients, and the outcomes are encouraging.
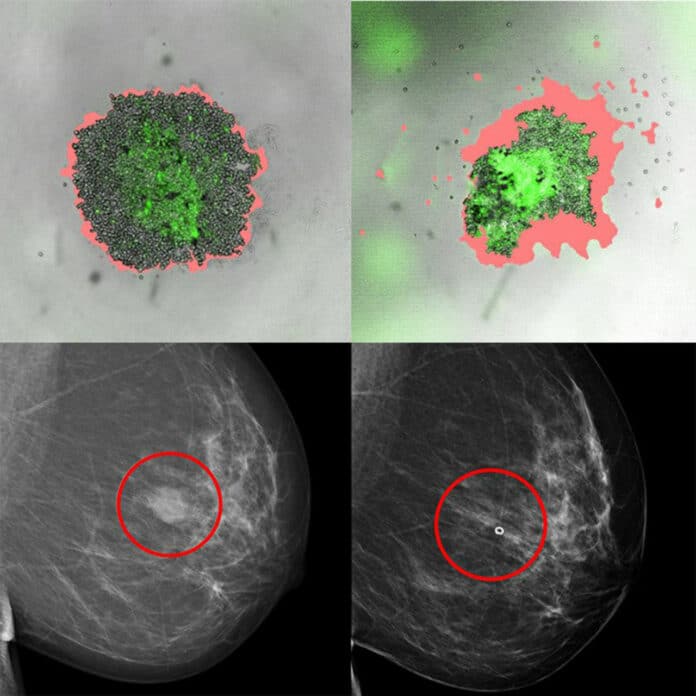
The method is based on isolating and cultivating tumor cells and so-called supporting cells from patients with breast cancer. The effectiveness of the cancer therapies is then evaluated by testing them on the cultivated cells at various concentrations.
The study has shown the possibility of establishing this type of cell-based tumor model from breast tumors and that the cell models are similar to the patients’ tumors of origin in relevant ways, for example, genetically and in terms of different protein markers.
The scientists developed tumor models for each patient using biopsies taken before surgery and subjected them to the same medications as the patient. The models’ pharmacological sensitivity was then contrasted with how patients responded to treatment.
The findings demonstrate that the therapeutic responses suggested by the tumor model and those that the patient subsequently displayed were broadly consistent. For instance, the model predicted the therapeutic response to the chemotherapy drug epirubicin with 90% accuracy, and four out of four patients who received treatment and underwent testing for anti-HER2 monoclonal antibody medications exhibited consistency.
The study’s first author Xinsong Chen, research specialist at the Department of Oncology-Pathology, Karolinska Institutet, said, “It is also possible to create cell models from small tumors, which are often considered technically challenging to sample without jeopardizing diagnostics, and that the tests can be carried out relatively quickly.”
“In most cases, we can perform individualized drug testing and get the result within ten days, indicating that this method can work in daily clinical practice. But it can also be used in research and drug development.”
The technology will then be tested in a broader sample of patients. Its potential to be combined with other molecular techniques will be looked at to improve therapy response prediction and research resistance mechanisms.
Journal Reference:
- X. Chen, E. G. Sifakis, S. Robertson, et al. 1668P – Breast cancer patient-derived whole-tumor cell culture model for efficient drug profiling and treatment response prediction. Proceedings of the National Academy of Sciences (PNAS). DOI: 10.1016/annonc/annonc1078