Almost all pediatric liver cancers were classified as either hepatoblastoma or hepatocellular carcinoma. But, pediatric pathologists observed that some liver cancer have histological features that do not fit into two carcinoma models. These cancers are less likely to respond to chemotherapy and poor patient outcomes.
The malignancies’ molecular profiles, including genetic changes and gene expression profiles, were investigated. According to the scientists, these profiles did not fall within the hepatoblastoma (HB) or hepatocellular carcinoma (HCC) molecular categories. Instead, these tumors had recurrent molecular characteristics seen in HBs and HCCs. These tumors were labeled as hepatoblastomas with hepatocellular carcinoma characteristics (HBCs).
Scientists also looked at HBC treatments and outcomes. They found that the treatments and results were more resistant to traditional chemotherapy and had poor outcomes if they weren’t treated with more aggressive surgical techniques, such as transplantation.
Scientists devised a diagnostic algorithm to stratify HBCs and guide specialized treatment based on the findings.
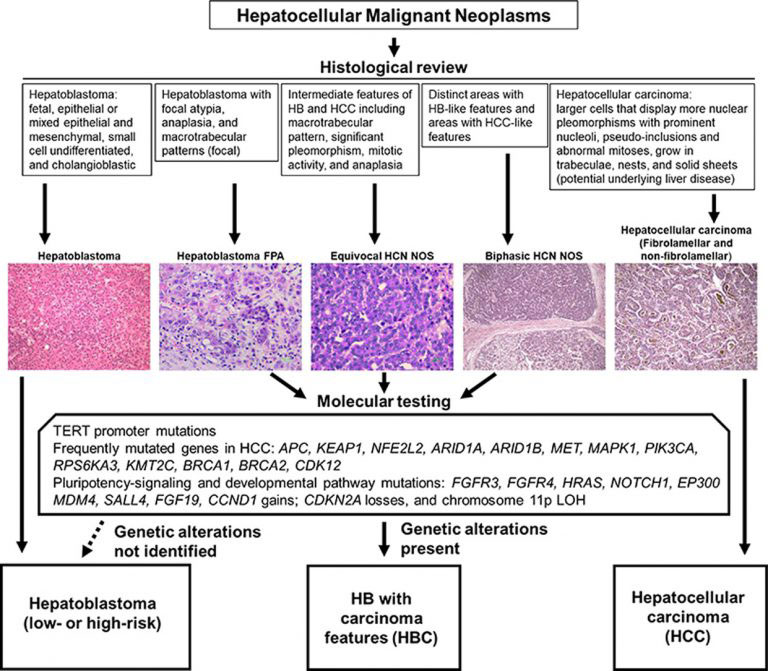
Dr. Dolores López-Terrada, corresponding author of the paper, professor of pathology, immunology, and pediatrics at Baylor, and chief of the division of genomic medicine at Texas Children’s, said, “Our findings highlight the importance of molecular testing to accurately classify these tumors to optimize treatment recommendations at the time of initial diagnosis. Our analysis suggested that children with HBCs may benefit from treatment strategies that differ from the guidelines for patients with hepatoblastoma and hepatocellular carcinoma.”
Journal Reference:
- Pavel Sumazin, Tricia L. Peters et al. Hepatoblastomas with carcinoma features represent a biological spectrum of aggressive neoplasms in children and young adults. Journal of Hepatology, 2022; DOI: 10.1016/j.jhep.2022.04.035
