A team of McGill University clinician-scientists has recently confirmed a suspicion that doctors who work with people at risk of developing dementia have long suspected that patients who do not perceive they experience memory complications are at high risk of seeing their condition worsen in a short time frame.
In this, some brain conditions can meddle with a patient’s potential to comprehend that they have a medical difficulty, a neurological disorder known as anosognosia mostly associated with Alzheimer’s ailment.
In a study published today in Neurology, Dr. Pedro Rosa-Neto’s team from McGill’s Translational Neuroimaging Laboratory shows that people who experience this lack of awareness find a nigh threefold rise in the likelihood of developing dementia within two years.
Joseph Therriault, a master’s student in McGill’s Integrated Program in Neuroscience and lead author of the paper, analyzed 450 patients who gone through mild memory deficits but were still capable of taking care of themselves, who had been asked to rate their cognitive abilities. Close relatives of the patient likewise filled out the similar surveys. When a patient reported having no cognitive problems but the family member reported considerable difficulties, he was considered to have poor awareness of the illness.
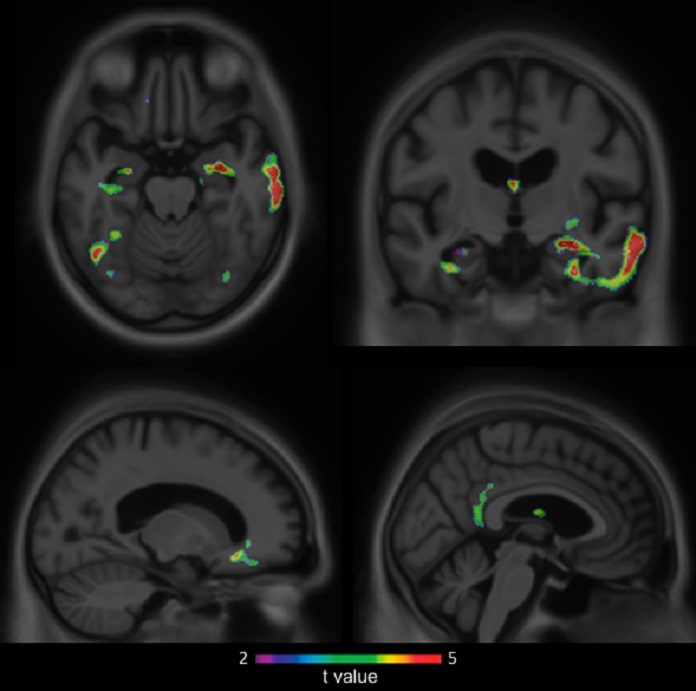
Later, researchers differentiated the poor awareness group to the ones demonstrated no awareness problems and discovered that those suffering from anosognosia had impaired brain metabolic function and higher rates of amyloid deposition, a protein known to accumulate in the brains of Alzheimer’s disease patients.
The previous study of two years later manifested that patients who were unaware of their memory problems were more likely to have developed dementia, even when taking into account other factors like genetic risk, age, gender, and education. The raised progression to dementia was mirrored by raised brain metabolic dysfunction in regions vulnerable to Alzheimer’s disease.
The finding- published in Neurology, provides crucial evidence about the prominent of consulting with the patient’s close family members during clinical visits.
Dr. Serge Gauthier, co-senior author of the paper and Professor of Neurology & Neurosurgery, Psychiatry, and Medicine at McGill said, “This has practical applications for clinicians: people with mild memory complaints should have an assessment that takes into account information gathered from reliable informants, such as family members or close friends.”
Dr. Rosa-Neto, co-senior author of the study and clinician scientist and director of the McGill Center for Studies in Aging, a research center affiliated with the Montreal West Island IUHSSC added, “This study could provide clinicians with insights regarding clinical progression to dementia.”
The scientists are recently taking this research further by exploring how awareness of illness changes across the full spectrum of Alzheimer’s ailment, and how these changes are related to critical Alzheimer’s biomarkers.