According to a new study by the University of Michigan, injecting nanoparticles aids to fight the immune system when it goes haywire. It can be done by redirecting invulnerable cells that reason aggravation far from damage site.
Inflammation can be said as a twofold edged sword. When it works, it enables the body to recuperate and wards off diseases. Be that as it may, now and then, the insusceptible framework blows up. Intense lung damage, maintained by breathing in smoke, for example, can prompt runaway liquid creation that basically suffocates a man.
Omolola Eniola-Adefeso, a professor of chemical engineering and biomedical engineering at U-M said, “Neutrophils are the first line of defense. They are the most active and the most optimized to mount an inflammatory response. They’re the underdogs of white blood cells, and we’re seeing that maybe we need to pay more attention to them.”
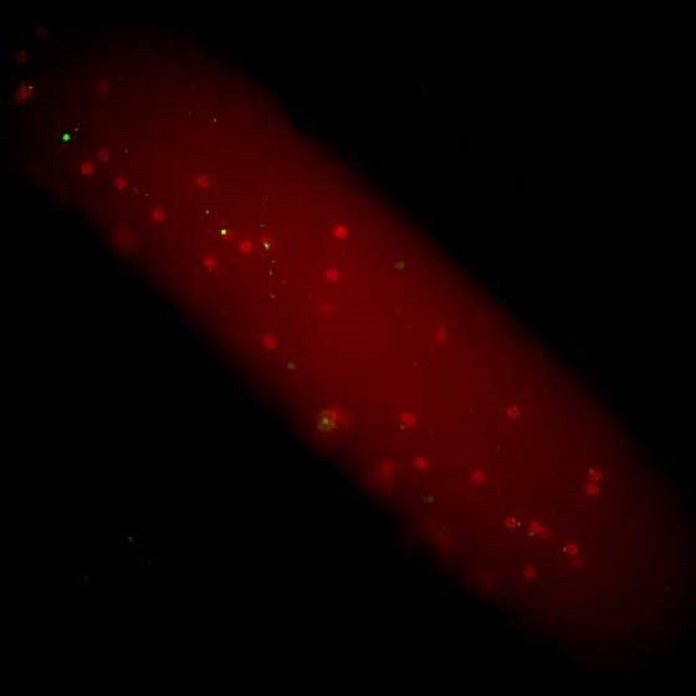
Scientists did their experiment with mice. Delivering simple plastic nanoparticles via IV might have the capacity to keep a sort of insusceptible cell—called a neutrophil—excessively caught up with, making it impossible to cause irritation. They started by exploring the dynamics within blood vessels. The dynamics help or hurt the ability of nanoparticles to deliver drugs to the blood vessel wall and beyond.
They observed the neutrophils were banishing their plastic particles, which were intended to join to the vein divider. This was an issue on the grounds that if the particles couldn’t tie, they couldn’t convey medications to infected tissue. However, in the wake of viewing the magnifying instrument video film commonly, they understood that the neutrophils additionally vanished—they weren’t official to the vein divider either.
Eniola-Adefeso said, “The ‘oh my God’ of horror about our particle turned into an excitement over these particles doing something to cells that had not previously been explored. These cool interactions between cells and particles got in the way of either one being able to do what they wanted to do.”
In next experiment, they confirmed that the neutrophils were redirecting their attention from creating inflammation at the injury site to carting the foreign particles away.
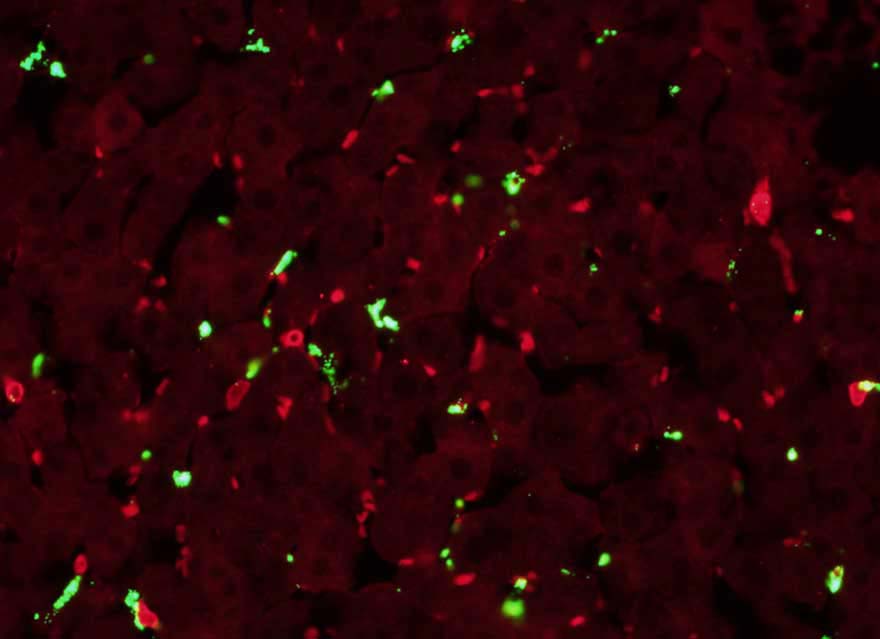
By using the technology that can see into the blood vessels of live mice, they identified mice with acute lung injury. They found that the infusing nanoparticles by IV could decrease neutrophils congregating at the damage site significantly or more.
The neutrophil concentration was the focus found in the blood of uninjured mice. Rather, the neutrophils were taking the particles to the liver, where they could be expelled from the flow.
Now, scientists want to figure out whether an injection of nanoparticles is a viable treatment for conditions with excessive inflammation.