Addiction is a disease that develops in stages: it starts with the initial exposure to a substance followed by a phase where consumption remains controlled. Some individuals, however, will start using drugs compulsively in spite of the major negative effects it has on their lives. Clinical estimates suggest that only one person in five moves from controlled to compulsive use.
What happens in the brain of a compulsive drug user? What is the difference in brain function between an addict and a person who takes a drug in a controlled manner?
To find out the answer to these questions, UNIGE scientists have observed the difference in the rodent addiction model. They found that the brain circuit connecting the decision-making region to the reward system is stronger in compulsive animals.
Christian Lüscher, senior author and professor at the Departments of Basic and Clinical Neurosciences of the Faculty of Medicine said, “We do not know why one person becomes addicted to drugs while another doesn’t. But our study identifies the difference in brain function between the two behaviors.”
As a model of addiction, the scientists embedded mice with an optic fiber, which empowered the animal to animate its reward system situated at the highest point of the brainstem. Pressing a little switch turned on a laser whose light enacted a molecular change recently added to nerve cells. The very same cells are initiated by addictive drugs and are in charge of the behavioral reinforcement.
Scientists also found that by decreasing the activity of this circuit, compulsive mice were able to regain control and that conversely, by stimulating the connection a mouse that initially remained in control became addicted.
Vincent Pascoli, the study’s lead author said, “We then introduce a weak electric shock so that we could observe, which mice continued with the self-stimulation. This allowed us to identify the mice that had become compulsive. Forty percent of the animals quickly stopped activating the lever following the introduction of the punishment. But 60% paid no heed to the negative consequences and continued to stimulate their reward system.”
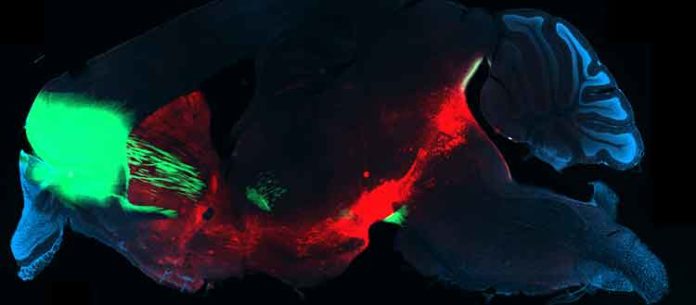
“When we used an optical technique to visualize the activity in the brain of freely moving mice. This uncovered a stronger activity in a circuit of addicted mice compared to mice that did not lose control. The circuit extends from the orbito-frontal cortex to the dorsal striatum, a part of the basal ganglia of the brain. The orbito-frontal cortex, located just above the eyes, is the region responsible for decision making.”
“This circuit was responsible for the compulsive behavior by artificially increasing its activity in a mouse that remained in control. The animal quickly developed a compulsive self-stimulation pattern. Conversely, when we reduced the activity of the circuit in an addicted mouse, she stopped activating the lever!”
Lüscher said “Given that the mice studied in the experiment were all genetically identical, how come the activity in the brain circuit was not the same for all of them? That’s the question we’ll try to answer in our future research.”
“Several hypotheses have been formulated, such as epigenetic contributions based on the life experiences that make each living being unique and influence the gene and brain function. Thanks to the present study, we now know which circuit causes the addiction. It will then be easier to find out what causes the disruption in the circuit.”
The work is published in this week’s edition of the journal Nature.