The Randomized Open Versus Robotic Cystectomy (RAZOR) preliminary indicated lower blood loss and blood transfusion rates and shorter hospital stays for patients who got an insignificantly intrusive medical procedure, however, there were no distinctions in complication rates and the two-year progression-free survival was almost the same.
This is the first far-reaching study contrasting the results of a robotic medical procedure with those of conventional open surgery in any organ. It has discovered that the medical procedures are similarly compelling in treating bladder growth.
A total of 350 patients were involved in the bladder cancer study. Half received the open surgical approach and half received robotic surgery, and they were followed for two to three years so that outcomes could be compared.
Dipen J. Parekh, M.D., chair of urology and director of robotic surgery at the University of Miami Miller School of Medicine said, “We have done more than 4 million surgeries with the robotic approach since the device came into existence, and on average we do close to a million robotic surgeries a year globally. There are close to 5,000 robotic systems installed all over the world – each one costs about $2 million – and yet until we did this study there was not a single Phase 3 multicenter randomized trial comparing this expensive new technology to the traditional open approach of doing surgeries.”
“No one had followed these patients over a period of time to find out if you are impacting their cancer outcomes with this robotic approach. We were able to prove unequivocally that we are not compromising patient outcomes by using robotic surgery.”
“The most important lesson from the study, Parekh said, is that more trials should be done, on other organs. It is possible to do well-designed Phase 3 multicenter surgical trials comparing new technology and surgical innovations to traditional ones before proclaiming superiority or success of one over the other. There’s a steep cost to robotic technology, and there is a learning curve, so we need to build on this in terms of making rational, data-based decisions.”
“Patients will also have more solid information as a result of this study and future research. The patients will ask better questions, and the physicians for the first time will be able to answer these questions, based on data rather than based on intuition. This is the highest level of data one can get.”
During the study, scientists asked patients about their quality of life at three and six months after surgery. All reported a significant return to their previous quality of life, there was no advantage of one group over the other.
Parekh said, “Some critics of robotic surgery have expressed concern about the lack of tactile feedback – an important guide in open surgery. When you do robotic surgery you don’t feel anything. It’s more by visual cues. If you’re doing open surgery you have the organs in your hands, you can feel them, and you assess and do these surgeries accordingly.”
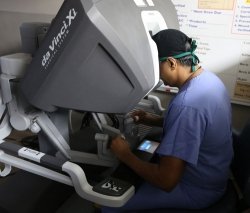
Parekh has extensive experience performing robotic surgeries with the da Vinci Xi Surgical System at UHealth Tower. It provides a magnified, three-dimensional view of the organs and a wide range of motion and flexibility. Robotic surgery has become particularly popular with prostate cancer patients – 90 percent of them choose it – which would make it difficult if not impossible to do a randomized study of surgical results in prostate cancer. But Parekh says that because robotic surgery is being used in many other organs, including kidney, colorectal, OB/GYN and lung cancer, more studies are needed.
And while there are improvements in perioperative recovery with robotic technology, operating room time is significantly longer for robotic surgery.
The seven-year study, conducted at 15 institutions, including Sylvester Comprehensive Cancer Center, and directed by Dipen J. Parekh, M.D., chair of urology and director of robotic surgery at the University of Miami Miller School of Medicine, is published in the June 23 issue of The Lancet.