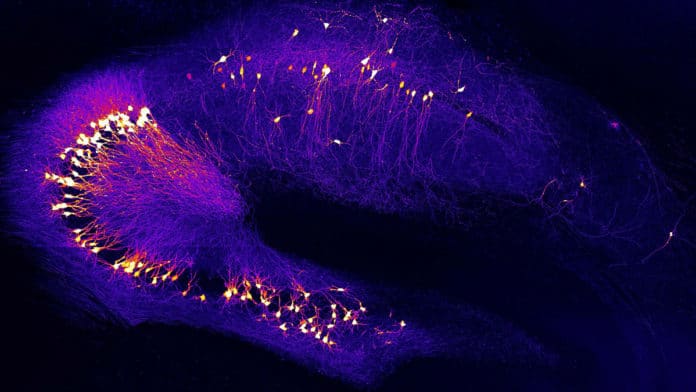
Hyperactive neurons in specific areas of the brain are accepted to be an early perturbation in Alzheimer’s disease. Now, scientists at the Technical University of Munich (TUM), for the first time, have recognized the cause of early cellular dysfunction in Alzheimer’s disease.
In a new study, scientists explained the reasons and mechanisms underlying this early and consequently significant neuronal dysfunction.
The brain of Alzheimer’s patients who have effectively created clinical symptoms contains enormous bunches of the protein beta-amyloid, known as plaques. Many therapeutic approaches focus on removing plaques. However, such endeavors have met with limited accomplishments to date.
During the study, scientists focused on hyperactive neurons, which occur at a very early stage – long before patients develop memory loss. As a consequence of hyperactivation, connected neurons in the circuits regularly receive false signals, leading to impairments in signal processing.

Image: A. Heddergott / TUM
Fascinatingly, scientists identified the cause and trigger of this early disturbance in the brain. They found that the excitatory neurotransmitter glutamate persists for too long near active neurons. This causes pathological overstimulation of those neurons – most likely contributing critically to impaired learning and memory loss in Alzheimer’s patients.
Neurons use a chemical called neurotransmitters for communication. Glutamate, one of the most significant of these chemicals, serves to actuate associated neurons. Glutamate is discharged at the interfacing site between two neurons, called synapses, and then quickly expelled to permit the transmission of the next signal. This removal includes supposed active siphon molecules just as a passive transport of glutamate along nearby membranes.
The specialists found that high concentrations of glutamate endured excessively long in the synaptic cleft of hyperactive neurons. This was because of the activity of beta-amyloid molecules, which shut glutamate transport out of the synaptic cleft. The group tried the component utilizing beta-amyloid atoms from patient examples and by using different mouse models obtaining comparable outcomes with the two approaches.
The team was also intrigued to discover that the neurotransmitter blockade was mediated by an early soluble form of beta-amyloid and not by the plaques. Beta-amyloid occurs initially as a single molecule form, or monomer, and then aggregates to double-molecule types (dimers) and larger chains resulting, eventually, in plaques. The researchers found that soluble dimers cause glutamate blockade.
Benedict Zott, the first author of the study, outlined, “Our data provide clear evidence for a rapid and direct toxic effect of a particular beta-amyloid type, the dimers. We were even able to explain this mechanism.”
The discovery is expected to open up a way to new therapeutic approaches and appeared in the journal Science.
Scientists now want to use this knowledge to improve further their understanding of the cellular mechanisms of Alzheimer’s and, thus, to support the development of strategies for treatment at the early stages of the disease.