Some coronary illness confronts a higher danger of sudden cardiovascular demise, which can happen when an arrhythmia—an unpredictable pulse—disturbs the typical electrical movement in the heart and makes the organ quit pumping. Be that as it may, arrhythmias connected to sudden cardiovascular demise are extremely uncommon, making it hard to examine how they happen—and how they may be avoided.
To make it easier to discover what causes these cardiac problems, scientists at the heart that precedes sudden cardiac death.
According to scientists, this digital model could give treatment focuses to sedate producers.
Raimond L. Winslow, the Raj & Neera Singh Professor of Biomedical Engineering at Johns Hopkins heart disease determine the probability of arrhythmias in cardiac tissue.”
“The importance of this is that we can now quantify precisely how these dysfunctions drive and influence the likelihood of arrhythmias. That is to say, we now have a way of identifying the most important controlling molecular factors associated with these arrhythmias.”
Scientists believe that the model could help them develop a treatment to keep some deadly heart rhythms from forming.
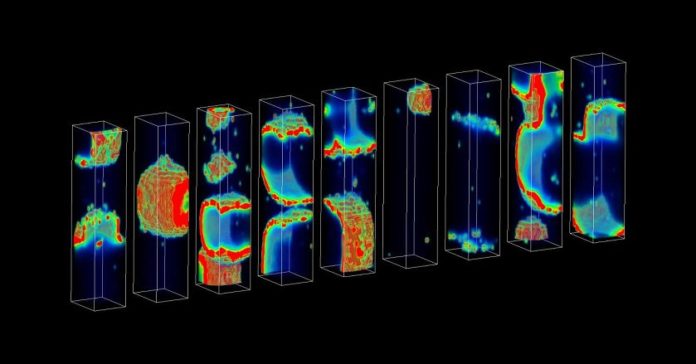
The model is somewhat like a rectangular structure, where each rectangle represents a heart cell in the team’s computer model.
The shading blasts portray spreading influxes of calcium. Every cell is indistinguishable however displays an unmistakable example of calcium waves because of arbitrary particle channel gating. The group examined how this arbitrariness offers to ascend to sudden capricious arrhythmias in cardiac problems.
Lead author of the study was Mark A. Walker said, “we used computer models to determine what action was linked to arrhythmia at three biological levels: in the heart tissue as a whole, within individual heart cells, and within the molecules that make up the cells, including small proteins called ion channels that control the movement of calcium in the heart.”
“Calcium is an important player in the functioning of a heart cell. There are a lot of interesting questions about how the handling of calcium in heart cells can sort-of go haywire.”
Scientists then started focusing on one fascinating inquiry regarding this procedure: when heart cells have excessive calcium, which can occur in coronary illness patients, how does this over-burden of calcium trigger an arrhythmia?
Scientists found that the heart cells react by ousting abundance calcium, and in doing as such, they produce an electrical flag. On the off chance that by shot, a sufficiently huge number of these signs are produced in the meantime, it can trigger an arrhythmia.
Walker said, “Imagine if you have a bunch of people in a room, and you want to test the strength of the floor they are all standing on. It’s not a very strong floor, so if there’s enough force on it, it will break. You tell everyone that on the count of three, jump in the air. They all land on the floor, and you try to figure out what’s the probability that the floor will break, given that everyone is going to jump at a slightly different time, people will weigh different amounts, and they might jump to different heights. These are all random variables.”
“Similarly, random variables also exist in trying to determine the probability that enough calcium-related electrical signals will simultaneously discharge in the heart to set off a lethal arrhythmia. Because the circumstances that cause sudden cardiac death are so rare, it makes them very tough to predict.”
Currently, the model cannot predict which heart patients face a higher risk of sudden cardiac death. But as scientists reported, the model should speed up the pace of heart research and the development of related medicines or treatments such as gene therapy.